OPTO-ACOUSTIC BREAST IMAGING
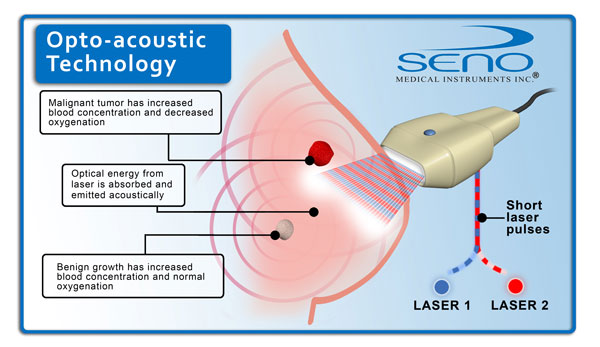
Opto acoustic breast imaging is a new generation diagnostic tool currently in the clinical trial stage for diagnosis of malignant or benign breast lumps. According to a European journal of breast cancer around 4 million new cases of breast cancer are detected every year with almost 80 percent of them turning out to be benign on laboratory testing. It is difficult for radiologists to rule out malignancy at the imaging stage. The cost of conducting surgical or core needle biopsy for every suspicious lump outweighs the results especially in women coming from struggling economies. A low cost diagnostic tool such as opto acoustic imaging can help in the timely detection of breast cancer in the early stages and also help prevent and control the increasing mortality due to this disease in developing as well as developed countries.
About Opto-Acoustic Breast Imaging: A Revolutionary Diagnostic Tool
Opto-acoustic breast imaging, also known as photo-acoustic imaging, is a cutting-edge advancement in medical imaging technology. This innovative tool is gaining significant attention for its ability to address many limitations of conventional ultrasound, especially in breast cancer detection and evaluation.
Why Opto-Acoustic Imaging Stands Out
While traditional ultrasound has long been a valuable resource in diagnosing a range of conditions, it primarily relies on the mechanical and elastic properties of tissues to generate image contrast. This approach can sometimes lead to ambiguous or inconclusive results. Opto-acoustic imaging, however, introduces a fundamentally different method by utilizing the light absorption properties of tissues, offering enhanced specificity and more accurate diagnostic capabilities.
“Opto-acoustic imaging offers a novel approach, leveraging light absorption to provide clearer, more detailed images, improving the accuracy of breast cancer diagnosis.”
Advantages of Opto-Acoustic Breast Imaging
- Enhanced Specificity: By focusing on the light absorption properties of tissues, opto-acoustic imaging provides clearer differentiation between normal and abnormal tissue structures.
- Improved Diagnostic Accuracy: This technology offers more precise imaging, which can lead to earlier and more accurate detection of breast cancer and other abnormalities.
- Overcoming Ultrasound Limitations: Unlike traditional ultrasound, which can sometimes produce inconclusive results due to its reliance on tissue elasticity, opto-acoustic imaging delivers more definitive diagnostic information.
Opto-acoustic imaging represents a significant leap forward in breast cancer diagnostics, offering a promising alternative to traditional imaging methods. As this technology continues to evolve, it holds the potential to become a standard tool in the early detection and management of breast cancer.
Understanding Conventional Ultrasound Technology
Conventional ultrasound technology operates by transmitting high-frequency sound waves into the body and interpreting the echoes that bounce back from different tissue types. These echoes are used to form an image, leveraging the mechanical differences between tissues—such as their stiffness or elasticity. While effective for many applications, this method often faces challenges in accurately differentiating between malignant and benign lesions in breast tissue. This limitation can lead to false positives or necessitate additional imaging studies.
Challenges in Breast Ultrasound Imaging
One significant issue with conventional ultrasound is its difficulty in penetrating dense breast tissue, which can obscure the clarity of images and make early cancer detection more challenging. Dense tissue can mask the presence of tumors, reducing the effectiveness of the ultrasound in identifying potential malignancies.
How Opto-Acoustic Imaging Overcomes These Challenges
Opto-acoustic imaging addresses the limitations of conventional ultrasound by incorporating laser-induced ultrasound technology. This advanced technique uses pulsed laser light directed into the tissue, where it is absorbed by molecules such as hemoglobin. The absorption of light energy causes a slight thermoelastic expansion in the tissue, generating ultrasound waves that are then detected and processed into highly detailed images.
“By combining laser-induced ultrasound with traditional methods, opto-acoustic imaging provides a clearer, more detailed view of breast tissue, particularly in dense areas.”
The Advantages of Opto-Acoustic Imaging
- Enhanced Tissue Differentiation: Opto-acoustic imaging exploits differences in light absorption between healthy and abnormal tissues, providing an additional layer of diagnostic information.
- Detailed Imaging: This technology offers highly detailed images that reveal critical indicators, such as the oxygenation and vascularization of tissues—key factors in cancer diagnostics.
- Improved Accuracy: By providing more precise information, opto-acoustic imaging reduces the likelihood of false positives and minimizes the need for follow-up imaging studies.
Opto-acoustic imaging represents a significant advancement in breast cancer diagnostics, particularly for patients with dense breast tissue. By offering a more accurate and comprehensive view, this technology holds promise for improving early detection and treatment outcomes.
Enhanced Specificity in Breast Lesion Evaluation
One of the standout advantages of opto-acoustic breast imaging is its ability to significantly enhance specificity when evaluating breast lesions. Traditional ultrasound often faces challenges in distinguishing between benign conditions, such as fibroadenomas, and malignant tumors. Both can present as solid masses with similar acoustic properties, making it difficult to differentiate between them.
Leveraging Optical Properties for Better Accuracy
Opto-acoustic imaging overcomes this challenge by analyzing the optical properties of breast tissue. Unlike conventional ultrasound, which relies solely on sound waves, opto-acoustic imaging can detect subtle differences in vascularization and oxygenation levels—two factors closely linked to tumor growth and malignancy.
“Tumors typically exhibit increased blood vessel formation (angiogenesis) and altered oxygen levels. Opto-acoustic imaging can visualize these changes with greater precision, leading to more accurate diagnoses.”
Reducing Unnecessary Procedures
- Improved Diagnostic Accuracy: By identifying specific changes in tissue oxygenation and blood flow, opto-acoustic imaging improves the accuracy of breast cancer diagnoses, reducing the uncertainty that often accompanies traditional ultrasound.
- Minimized Need for Biopsies: The enhanced specificity provided by opto-acoustic imaging reduces the need for unnecessary biopsies and follow-up imaging studies, streamlining the diagnostic process.
- Early Detection of Aggressive Tumors: Opto-acoustic imaging is particularly effective in detecting hypoxic regions within tumors, which are often associated with more aggressive forms of breast cancer. Early identification of these regions allows clinicians to tailor treatment plans more effectively, improving patient outcomes.
Overall, the ability to visualize differences in vascularization and oxygenation levels makes opto-acoustic imaging a powerful tool in breast cancer diagnostics. By offering greater specificity and accuracy, this technology not only enhances diagnostic confidence but also helps to avoid unnecessary procedures, leading to better patient care.
Effectiveness in Dense Breast Tissue
One of the standout advantages of opto-acoustic breast imaging is its ability to perform effectively in patients with dense breast tissue. Dense tissue often presents challenges for traditional mammography and ultrasound because it appears white on a mammogram—similar to how potential tumors appear—making it difficult to detect abnormalities. Opto-acoustic imaging bypasses this issue by focusing on the optical properties of tissues rather than their density, enabling clearer visualization of suspicious areas, particularly in patients with dense breasts.
Non-Invasive and Radiation-Free Imaging
Another critical benefit of opto-acoustic imaging is its non-invasive nature and the absence of ionizing radiation, making it a safer alternative to other imaging modalities such as mammography and CT scans. This aspect is especially important for younger patients or those requiring frequent imaging, as repeated exposure to ionizing radiation can increase the risk of developing cancer.
“Opto-acoustic imaging provides a safer alternative by eliminating radiation exposure, making it ideal for patients who need regular monitoring.”
Complementary Use with Traditional Ultrasound
- Enhanced Visualization: Opto-acoustic imaging excels in detecting abnormalities in dense breast tissue, where traditional methods may struggle.
- Safety and Non-Invasiveness: The technique is non-invasive and free from ionizing radiation, reducing the long-term risks associated with repeated imaging.
- Complementary Diagnostics: Opto-acoustic imaging can be used alongside traditional ultrasound, offering a complementary approach that enhances the overall diagnostic process.
By combining opto-acoustic imaging with traditional ultrasound, healthcare providers can improve the accuracy and safety of breast cancer diagnostics, particularly in challenging cases involving dense breast tissue. This combined approach ensures that patients receive the most comprehensive and effective care possible.
Opto-Acoustic Imaging: Beyond Detection
As research advances, opto-acoustic imaging is proving to be valuable not only in breast cancer detection but also in monitoring treatment responses. By evaluating changes in tissue oxygenation and blood flow, this technology enables clinicians to assess how tumors are responding to therapies such as chemotherapy or radiation. This real-time monitoring capability is crucial for personalizing treatment plans, allowing healthcare providers to adjust interventions based on the effectiveness of the ongoing therapy.
Emerging Technology with Growing Potential
Despite its numerous advantages, opto-acoustic imaging is still an emerging technology and is not yet widely available in clinical settings. However, ongoing clinical trials and research are paving the way for its broader adoption. Researchers are continually refining the technology to improve its sensitivity and accuracy, as well as exploring ways to integrate it with other imaging modalities for a more comprehensive diagnostic approach.
“Opto-acoustic imaging represents the future of breast cancer diagnostics, with the potential to revolutionize how we detect and monitor this disease.”
Clinical Trials and Future Applications
- Treatment Monitoring: Opto-acoustic imaging allows for the assessment of tissue oxygenation and blood flow, making it a powerful tool for monitoring how well a tumor responds to treatments.
- Personalized Care: This real-time feedback can help tailor treatment plans, ensuring that interventions are adjusted based on a patient’s unique response.
- Broadening Access: As clinical trials continue and research progresses, the technology is expected to become more widely available, offering enhanced diagnostic capabilities in routine clinical practice.
In conclusion, opto-acoustic breast imaging offers a groundbreaking approach to both diagnosing and monitoring breast cancer. By leveraging the optical properties of tissues, it enhances diagnostic specificity, minimizes the need for invasive procedures, and provides safer, radiation-free imaging. As this technology evolves, it holds tremendous promise for improving early detection rates and enabling more personalized treatment plans for breast cancer patients.
Understanding Opto-Acoustic Imaging: Exploring Laser-Induced Ultrasound Technology
Opto-acoustic imaging, also known as photo-acoustic imaging, is a revolutionary diagnostic technique that uses laser-induced ultrasound waves to produce highly detailed images of tissues. This advanced approach works on the principle that specific tissues, when exposed to particular wavelengths of light, absorb that light and emit sound waves. These sound waves are then captured and processed to create images that offer a remarkably clear view of the body’s internal structures.
How Does Opto-Acoustic Imaging Work?
The key to opto-acoustic imaging lies in its ability to detect and identify various chromophores—molecules that absorb light at specific wavelengths and play a crucial role in determining imaging contrast. Important chromophores in biological tissues include:
- Hemoglobin: Absorbs light at specific wavelengths, providing insights into blood vessel structure and oxygenation levels.
- Lipids: These are fats that absorb light differently, helping to distinguish between different types of tissues.
- Water: A key component in tissues, water absorbs light in unique patterns that aid in imaging clarity.
Each of these substances has a distinct absorption spectrum, meaning they absorb light at different wavelengths. This characteristic allows opto-acoustic imaging to differentiate between tissue types more effectively than traditional ultrasound, which relies primarily on mechanical properties like tissue density and elasticity.
Advantages Over Traditional Ultrasound
“Opto-acoustic imaging not only enhances tissue differentiation but also provides a new dimension to diagnostic imaging by leveraging the unique optical properties of tissues.”
While traditional ultrasound is valuable for many applications, it can sometimes struggle to distinguish between different tissue types. Opto-acoustic imaging, by contrast, offers:
- Enhanced Contrast: By using light absorption characteristics, this technique provides better differentiation between tissues.
- Detailed Vascular Imaging: The ability to visualize blood vessels and their oxygenation levels can be crucial for cancer diagnostics.
- Non-Invasive: Similar to traditional ultrasound, opto-acoustic imaging is non-invasive and does not require ionizing radiation.
In summary, opto-acoustic imaging represents a significant advancement in medical imaging technology. By utilizing the optical properties of tissues, it offers enhanced specificity and accuracy, particularly in challenging diagnostic areas like breast cancer detection. As this technology continues to evolve, it promises to become an invaluable tool in clinical settings, providing healthcare professionals with a powerful method for early diagnosis and treatment planning.
Exploring the Advantages of Opto-Acoustic Imaging
Opto-acoustic imaging, also known as photo-acoustic imaging, is a groundbreaking technology that enhances medical diagnostics by taking advantage of the unique properties of hemoglobin, which is abundant in blood. Hemoglobin has the ability to absorb light in the near-infrared spectrum. When targeted by a laser, this absorption generates an acoustic signal that can be detected and used to:
- Map Blood Vessels: Opto-acoustic imaging provides detailed maps of blood vessels, helping clinicians visualize the vascular structure in unprecedented detail.
- Identify Abnormal Vascularization: This technology excels at detecting abnormal blood vessel formation, which is often associated with various diseases, including cancer.
- Assess Oxygenation Levels: By analyzing oxygen levels within tissues, opto-acoustic imaging offers critical insights into tissue health and the presence of disease.
“These capabilities are particularly valuable in oncology, where tumor angiogenesis—the formation of new blood vessels—is a key indicator of malignancy and tumor growth.”
Opto-acoustic imaging, therefore, provides crucial insights into tumor biology that might be overlooked by conventional imaging techniques. By visualizing the formation of new blood vessels, which is often a sign of aggressive tumor growth, this technology offers a deeper understanding of cancer progression. This enhanced diagnostic capability allows for more accurate assessments, enabling clinicians to tailor treatments more effectively.
Deeper Penetration and Enhanced Detection
“Opto-acoustic imaging excels in achieving greater penetration depths, making it possible to visualize structures several centimeters beneath the surface, a capability that purely optical techniques struggle with.”
One of the most significant advantages of opto-acoustic imaging over purely optical imaging modalities is its superior ability to penetrate deeper into tissues. Traditional techniques like optical coherence tomography (OCT) rely on ballistic photons—light particles that travel through tissues. However, these photons scatter rapidly when encountering dense or heterogeneous tissues, limiting the imaging depth to just a few millimeters.
Opto-acoustic imaging overcomes this limitation by utilizing ultrasound waves generated through light absorption. This approach allows for the visualization of structures located several centimeters beneath the surface, making it an invaluable tool in medical diagnostics.
- Breast Imaging: This deeper penetration capability is particularly beneficial for breast imaging, where examining tissues that lie deeper within the breast is often necessary, especially in women with dense breast tissue. The ability to visualize these deeper structures helps in detecting abnormalities that might otherwise go unnoticed with conventional imaging techniques.
- Diverse Applications: Beyond breast imaging, opto-acoustic technology’s enhanced penetration depth makes it applicable in various medical fields where deep tissue visualization is crucial, further expanding its diagnostic potential.
Enhanced Breast Imaging for Dense Tissue
Breast tissue, particularly in women with dense breasts, can obscure potential abnormalities, making detection challenging with traditional modalities like mammography or ultrasound. Opto-acoustic imaging, however, allows for deeper penetration and provides clearer images of the entire breast, including areas that may be difficult to access with conventional techniques. This improved visualization is crucial for early detection and accurate diagnosis.
Specificity in Chromophore Differentiation
The ability of opto-acoustic imaging to differentiate between various chromophores in breast tissue adds an additional layer of specificity to the imaging process. For example, it can distinguish between oxygenated and deoxygenated hemoglobin, which is vital for assessing tumor hypoxia—a condition where cancerous tissues are deprived of adequate oxygen. Tumor hypoxia is a well-known marker of aggressive cancers and poor prognosis. By identifying hypoxic regions within a tumor, opto-acoustic imaging can help clinicians tailor treatment strategies to effectively address more aggressive cancer subtypes.
Non-Invasive and Radiation-Free Imaging
Another important advantage of opto-acoustic imaging is its non-invasive nature and lack of ionizing radiation. Techniques like mammography expose patients to low doses of radiation, which, while generally safe, can accumulate over time, especially in individuals who require frequent imaging. Opto-acoustic imaging, on the other hand, uses harmless laser pulses and ultrasound waves, making it a safer option for long-term monitoring and routine breast cancer screenings, particularly in younger patients or those with a high risk of developing breast cancer.
Conclusion: Opto-Acoustic Imaging’s Role in Modern Diagnostics
Opto-acoustic imaging represents a powerful tool in the diagnostic arsenal, offering deeper tissue penetration, enhanced specificity in detecting vascularization and hypoxia, and the added benefit of being non-invasive and free of ionizing radiation. As this technology continues to advance, it is poised to play a critical role in improving early detection rates and providing more personalized treatment options for breast cancer and other conditions.
Expanding Applications of Opto-Acoustic Technology
Opto-acoustic technology, initially focused on breast imaging, is rapidly gaining traction across various medical fields due to recent advancements. Researchers are now exploring its potential in several key areas, highlighting its versatility and broad impact.
Key Areas of Application
- Cardiology: Opto-acoustic imaging is being studied for its ability to visualize blood flow and detect atherosclerotic plaques. This non-invasive technique could revolutionize how cardiovascular diseases are diagnosed and monitored, providing detailed images of blood vessels and plaque formations.
- Dermatology: In the realm of skin cancer, opto-acoustic imaging offers a detailed view of vascular networks within lesions, helping to distinguish between benign and malignant growths. This capability enhances the accuracy of skin cancer assessments and may reduce the need for invasive biopsies.
For a deeper dive into opto-acoustic imaging in cardiology, you can explore this research article on its use in detecting atherosclerotic plaques.
Opto-Acoustic Imaging in Precision Medicine
“As opto-acoustic imaging evolves, it is poised to become a cornerstone in precision medicine, offering real-time insights into the molecular and vascular characteristics of tissues.”
The role of opto-acoustic imaging in precision medicine is becoming increasingly significant. This technology provides real-time data on the molecular and vascular properties of tissues, enabling clinicians to make more informed decisions about diagnosis, treatment planning, and therapeutic monitoring.
In breast cancer treatment, for example, opto-acoustic imaging can monitor changes in tumor oxygenation levels during chemotherapy. By tracking these changes, physicians can adjust treatment regimens in real-time, improving the effectiveness of the therapy and potentially leading to better patient outcomes.
As the technology continues to evolve, opto-acoustic imaging is expected to be integrated more deeply into clinical practice, offering new ways to enhance patient care across a variety of medical disciplines. Stay updated with the latest advancements in this field by visiting our Rad Tech Talk section.
The Future of Opto-Acoustic Imaging
In conclusion, opto-acoustic imaging represents a groundbreaking advancement in medical diagnostics by combining the strengths of optical and acoustic technologies. Its ability to visualize deep tissue structures, distinguish between different chromophores, and provide functional information about tissue oxygenation makes it an invaluable tool not only in breast imaging but across various medical fields. As this technology continues to mature and gain wider adoption, it has the potential to significantly enhance early detection, reduce the need for unnecessary biopsies, and improve patient outcomes across a broad spectrum of medical disciplines.
Real-Time Physiological Monitoring with Opto-Acoustic Imaging: Enhancing Breast Cancer Diagnostics
One of the most groundbreaking features of opto-acoustic imaging is its ability to provide real-time functional data on key physiological parameters such as tissue temperature, blood flow, and oxygenation levels. This advanced diagnostic tool detects subtle changes in the optical properties of tissues, which occur due to physiological or pathological processes. By capturing these variations, opto-acoustic imaging offers a dynamic view of tissue health, making it especially useful for detecting abnormalities linked to conditions like cancer.
Mapping Oxygenated and Deoxygenated Blood in Real Time
- Oxygen Mapping: Clinicians can use opto-acoustic technology to track the distribution and concentration of oxygenated versus deoxygenated blood in tissues, providing critical insights into tumor biology.
- Tumor Vascularization: Malignant tumors often exhibit abnormal patterns of blood flow and oxygenation. By identifying these patterns, opto-acoustic imaging can pinpoint hypoxic regions—areas of the tumor deprived of oxygen due to poor blood supply.
“Hypoxic regions in tumors are often associated with more aggressive cancer types, resistance to treatment, and poor prognosis.” – National Institutes of Health
This ability to detect hypoxia, or low oxygen levels, is critical because hypoxic areas within tumors often correlate with aggressive cancer behavior and treatment resistance. By identifying these regions, opto-acoustic imaging helps guide more tailored therapeutic decisions, enhancing the precision of cancer treatment.
Improving Diagnostic Accuracy: Differentiating Between Benign and Malignant Lesions
While traditional imaging methods like mammography and ultrasound can identify suspicious masses, they often lack the specificity needed to determine whether a lesion is benign or malignant. This frequently leads to invasive biopsies for diagnostic confirmation. Opto-acoustic imaging offers an alternative by non-invasively assessing the vascular and metabolic characteristics of breast lesions.
Key Diagnostic Advantages of Opto-Acoustic Imaging
- Angiogenesis Detection: Malignant tumors typically develop abnormal blood vessel networks, a process known as angiogenesis. Opto-acoustic imaging can visualize these vascular changes, helping to distinguish between cancerous and non-cancerous lesions.
- Oxygenation Profiles: Opto-acoustic imaging can reveal altered oxygenation patterns in tumors, offering additional clues about malignancy that traditional methods may miss.
By identifying these unique vascular signatures, opto-acoustic imaging can significantly reduce the need for unnecessary biopsies, helping clinicians make more informed, non-invasive diagnoses. Learn more about how this technology is transforming cancer diagnostics by visiting Rad Tech Talk.
Opto-Acoustic Imaging: A Breakthrough in Breast Cancer Diagnostics
As clinical trials continue to evaluate the effectiveness of opto-acoustic imaging in breast cancer diagnostics, early results are highly promising. This cutting-edge technology has the potential to significantly enhance early detection, improve diagnostic accuracy, and reduce patient discomfort, all while minimizing healthcare costs. Below, we’ll break down the exciting capabilities of opto-acoustic imaging and explore its future impact on cancer care.
Key Advantages of Opto-Acoustic Imaging
- Enhanced Early Detection: Opto-acoustic imaging provides greater specificity than conventional imaging techniques by utilizing the light absorption properties of tissues, allowing for more accurate identification of malignant lesions.
- Reduced Patient Discomfort: As a non-invasive imaging modality, opto-acoustic imaging minimizes the need for invasive biopsies, leading to less patient discomfort and reduced recovery times.
- Lower Healthcare Costs: By potentially reducing the number of unnecessary procedures, such as biopsies, this technology could help lower overall healthcare expenses.
Real-Time Monitoring of Tumor Response
“One of the most exciting prospects of opto-acoustic imaging is its ability to monitor tumor responses to treatment in real time.”
Opto-acoustic imaging stands out by offering real-time feedback on how tumors respond to treatments like chemotherapy or radiation. By tracking changes in tissue oxygenation and blood flow, clinicians can assess the effectiveness of these therapies early in the treatment process. This capability allows doctors to adjust treatments as needed, potentially preventing significant tumor progression and tailoring therapy to individual patient needs.
Broader Oncology Applications
Beyond breast cancer diagnosis, opto-acoustic imaging is poised to revolutionize oncology by offering non-invasive monitoring of tumor metabolism and vascular health. This feature is particularly valuable for managing metastatic disease, where real-time imaging of multiple tumor sites is essential to assess cancer spread and activity throughout the body.
Expanding Beyond Oncology: Cardiovascular Applications
Opto-acoustic imaging’s ability to visualize and quantify changes in blood flow and oxygenation also holds promise in other medical fields, particularly cardiology. In cardiology, the technology could be used to assess tissue perfusion, which is critical for diagnosing and managing heart disease. By providing detailed real-time images of blood flow, opto-acoustic imaging could help identify heart conditions earlier and more accurately.
Integrating Opto-Acoustic Imaging into Clinical Practice
While still in the clinical trial phase, opto-acoustic imaging is on track to become a game-changer in routine clinical practice. As research advances, combining opto-acoustic imaging with traditional diagnostic tools like ultrasound or mammography could result in more comprehensive imaging protocols that enhance diagnostic confidence. This would reduce patient anxiety and the need for unnecessary invasive procedures.
Impact on Personalized Cancer Care
The real-time data that opto-acoustic imaging provides on blood flow, oxygenation, and tissue metabolism brings a new level of precision to breast cancer diagnostics. This technology offers an opportunity to reduce the number of invasive biopsies, streamline diagnostic workflows, and ultimately improve patient outcomes.
“As clinical trials continue to demonstrate its efficacy, opto-acoustic imaging is poised to become an integral part of personalized cancer care, helping clinicians deliver more precise and effective treatments.”
Opto-acoustic imaging is an exciting development in the field of personalized cancer care. By delivering real-time, detailed insights into tumor behavior, this technology has the potential to revolutionize how cancer is diagnosed and treated. Stay updated on the latest advancements by visiting our Rad Tech Talk section for more insights.
Laser Wavelengths in Opto-Acoustic Imaging
In opto-acoustic imaging, laser wavelengths from the visible to near-infrared (NIR) spectrum, typically ranging between 550 and 900 nm, are used to penetrate tissues. The NIR range, particularly between 600 and 900 nm, offers the deepest penetration, reaching several centimeters into the tissue. This depth is crucial for effective breast tissue imaging, allowing clinicians to visualize structures deep beneath the surface that are difficult to assess with traditional techniques like mammography or ultrasound.
Advantages of Deep Penetration in Dense Breast Tissue
- Enhanced Clarity: Dense breast tissue can obscure tumors on standard mammograms, but opto-acoustic imaging reveals deeper abnormalities with greater clarity and precision.
- Improved Tumor Detection: Tumors in dense breast tissue are more easily visualized due to the deeper penetration of the laser wavelengths, allowing for earlier detection and evaluation.
“The ability to reach deeper tissue layers is critical for assessing areas where traditional imaging methods struggle, particularly in patients with dense breast tissue.”
Detection and Evaluation of Breast Lumps
One of the unique strengths of opto-acoustic imaging is its capacity to observe physiological changes in real-time, providing crucial insights into whether a breast lump is benign or malignant. Tumors often alter the vasculature in the surrounding tissue, leading to abnormal blood flow and oxygenation levels.
Functional and Anatomical Benefits
- Real-Time Blood Flow Observation: Opto-acoustic imaging allows healthcare providers to monitor changes in blood flow, helping to detect malignancy based on how tumors affect surrounding vasculature.
- Vascular Mapping: The technology can also identify angiogenesis, the formation of new blood vessels, which is often a sign of aggressive cancers.
- High-Resolution Anatomical Images: The combination of real-time functional data with detailed anatomical images enhances the accuracy of breast lump evaluation.
“Mapping vascular changes such as angiogenesis is particularly valuable in identifying aggressive cancers that may not be easily visible with other imaging techniques.”
Reducing Unnecessary Biopsies
Opto-acoustic imaging holds significant promise as a non-invasive, cost-effective alternative to invasive biopsies. While it may not be intended as a first-line screening tool like mammograms, it has the potential to reduce the need for unnecessary biopsies.
Benefits of Opto-Acoustic Imaging over Biopsies
- Non-Invasive: This technology offers a non-invasive method to assess breast lesions, reducing the need for tissue sampling.
- High Accuracy: Opto-acoustic imaging provides high-accuracy data, helping physicians determine the likelihood of malignancy without biopsy.
- Reduced Risks and Costs: Biopsies are costly, time-consuming, and carry risks like infection or discomfort. Opto-acoustic imaging offers a safer, more affordable alternative.
“Opto-acoustic imaging could significantly reduce the emotional and financial burden on patients who undergo unnecessary biopsies after suspicious findings on traditional imaging tests.”
Opto-Acoustic Breast Imaging: A Promising Tool in Breast Cancer Detection
Opto-acoustic breast imaging, although still in the clinical trial phase, is demonstrating significant potential in reducing breast cancer-related mortality worldwide. This cutting-edge technology provides highly detailed imaging of both the anatomy and physiology of breast tissue, which can lead to earlier detection and more accurate diagnosis of breast cancer. Early detection is crucial, as it greatly increases the chances of successful treatment and long-term survival. Furthermore, the real-time capabilities of opto-acoustic imaging enable physicians to monitor tumor responses to treatments like chemotherapy or radiation, enhancing personalized patient care.
Real-Time Functional Data and Anatomical Imaging
“Opto-acoustic imaging offers a comprehensive view of tissue oxygenation, blood flow, and metabolic activity in addition to anatomical details, making it a powerful diagnostic tool.”
One of the most compelling aspects of opto-acoustic imaging is its ability to provide real-time data on critical physiological parameters such as:
- Tissue oxygenation
- Blood flow
- Metabolic activity
This data, combined with high-resolution anatomical imaging, allows healthcare providers to gain a deeper understanding of the biological behavior of breast tumors. By offering insights into these functional characteristics, opto-acoustic imaging supports more accurate diagnoses and helps physicians tailor personalized treatment plans for patients.
Tracking Tumor Hypoxia for Better Treatment Outcomes
Opto-acoustic imaging is especially useful in identifying tumor hypoxia—a condition where parts of a tumor are deprived of oxygen. Tumors that exhibit hypoxia are often more resistant to standard treatments like chemotherapy or radiation, which can result in poor patient outcomes. By detecting these hypoxic regions early, clinicians can adjust treatment plans to specifically target these aggressive cancer subtypes, ultimately improving the efficacy of therapies and patient prognosis.
Cost-Effective Alternative to Invasive Procedures
A significant advantage of opto-acoustic imaging is its potential to reduce the need for invasive procedures like biopsies. Biopsies, while critical for diagnosis, come with risks such as infection, patient discomfort, and high costs. Opto-acoustic imaging offers a non-invasive alternative that provides high diagnostic confidence, potentially minimizing the need for these follow-up procedures. This not only reduces the emotional and physical burden on patients but also lowers overall healthcare costs.
Streamlining Cancer Diagnostics
Traditional imaging techniques, such as mammograms, often require follow-up biopsies to confirm suspicious findings. However, opto-acoustic imaging can help reduce the number of unnecessary biopsies by providing more detailed information about the biological characteristics of breast tissue. By visualizing blood flow and metabolic activity, opto-acoustic imaging offers a clearer picture of whether a breast lump is likely to be malignant or benign. This streamlined diagnostic process can lead to more efficient healthcare delivery, reducing patient anxiety and speeding up treatment decisions.
Conclusion: A Game-Changer in Breast Cancer Care
“With its ability to deliver real-time, non-invasive imaging of both anatomy and tissue function, opto-acoustic technology is poised to revolutionize breast cancer diagnostics and treatment.”
The Future of Opto-Acoustic Imaging
As clinical trials advance, the potential of opto-acoustic imaging in breast cancer care looks promising. By integrating the capabilities of functional and anatomical imaging, this cutting-edge technology could significantly improve early detection rates, reduce the number of unnecessary biopsies, and enhance patient outcomes. With its ability to offer non-invasive, real-time imaging, opto-acoustic imaging is expected to play a pivotal role in the future of breast cancer diagnostics.
Key Benefits of Opto-Acoustic Imaging
- Early Detection: This technology allows for the early identification of breast tumors, potentially leading to faster diagnosis and treatment.
- Non-Invasive: Unlike traditional biopsies, opto-acoustic imaging offers a non-invasive alternative, reducing patient discomfort and procedural risks.
- Cost-Effective: By minimizing unnecessary biopsies and follow-up procedures, opto-acoustic imaging could help lower healthcare costs.
- Real-Time Data: Clinicians gain real-time insights into tumor behavior, including blood flow, oxygenation, and metabolic activity, allowing for more personalized treatment plans.
Opto-Acoustic Imaging in Precision Medicine
As the technology continues to develop, its application in precision medicine is expected to grow. Opto-acoustic imaging provides detailed insights into the molecular and vascular characteristics of breast tissue, enabling more accurate diagnoses and treatment planning. For example, it can help identify hypoxic regions within tumors—areas with low oxygen levels—which are often more resistant to treatment. By detecting these aggressive cancer subtypes, physicians can adjust therapies for improved effectiveness.
A Global Impact in Breast Cancer Care
Opto-acoustic imaging has the potential to revolutionize breast cancer care globally. Its detailed, real-time visualization of breast tissue can empower healthcare providers with the information needed to make more accurate diagnoses. As research progresses, this technology could become a critical tool for reducing mortality rates and improving treatment outcomes for breast cancer patients worldwide.
Short Background: The Science Behind Opto-Acoustic Imaging
“Opto-acoustic imaging combines light and sound to offer a multi-dimensional view of internal structures, enhancing both anatomical and functional imaging.”
How Opto-Acoustic Imaging Works
Opto-acoustic imaging is a cutting-edge diagnostic technique that blends optical imaging with the precision of ultrasound. This powerful technology provides exceptional detail by visualizing internal structures while also offering functional insights. The key to its effectiveness lies in using short pulses of infrared light to generate ultrasound waves within the body, which makes it a unique fusion of light and sound.
The Infrared Light Advantage
- Non-Ionizing Light: Opto-acoustic imaging uses near-infrared (NIR) light, which is safe and non-ionizing, making it ideal for imaging sensitive areas like the breast.
- Deep Penetration: Unlike traditional optical imaging, NIR light penetrates several centimeters deep into tissues, allowing for more thorough imaging of dense structures, such as breast tissue.
Chromophore Interaction and Sound Wave Generation
As the infrared light interacts with tissues, it is absorbed by specific molecules, known as chromophores, such as hemoglobin, water, and lipids. This absorption causes slight thermoelastic expansion, which generates sound waves. These sound waves vary in intensity depending on the tissue’s composition and the chromophores’ optical absorption properties. For example:
- Oxygenated vs. Deoxygenated Blood: Tissues with high oxygenated blood concentrations emit different acoustic signals compared to deoxygenated or dense fibrous tissues.
- Vascular Insights: This difference in acoustic signals allows for detailed information on blood flow and oxygenation levels, which are crucial for tumor detection and evaluation.
Data Capture and Image Creation
Once the sound waves are produced, they are captured by a highly sensitive transducer placed over the area being examined—such as the breast. This transducer functions similarly to a traditional ultrasound transducer by converting acoustic signals into electrical signals. The imaging system processes this data to generate detailed images, offering both structural and functional views of the tissue.
Multi-Dimensional View: Beyond Structure
Opto-acoustic imaging delivers a multi-dimensional perspective, combining structural and functional imaging. Clinicians can not only observe the physical arrangement of tissues but also assess their metabolic and vascular activity. This makes it a powerful tool for detecting abnormalities like tumors, which often exhibit distinct blood flow and oxygenation patterns.
For more in-depth information on opto-acoustic technology, you can explore related resources like the 3D Breast Ultrasound or visit NCBI for further research on chromophore absorption.
Functional Insights: What Sets Opto-Acoustic Imaging Apart
“The ability to visualize tissue functionality is what makes opto-acoustic imaging stand out from traditional imaging modalities.”
Beyond Detection: Functional Assessment
While conventional mammography and ultrasound can identify the presence of a mass or lesion, they often fall short in determining whether that mass is malignant or benign without further testing, such as a biopsy. Opto-acoustic imaging, on the other hand, provides real-time functional data that can help differentiate between cancerous and non-cancerous tissues. Here’s how:
- Blood Flow and Oxygenation: Malignant tumors tend to have abnormal patterns of blood vessel growth (angiogenesis) and altered oxygen metabolism.
- Sound Wave Intensity: Opto-acoustic imaging detects these abnormalities by analyzing variations in the intensity of sound waves generated by the tissue, offering a non-invasive assessment of suspicious lesions.
Advantages in Spatial Resolution and Penetration Depth
Another standout feature of opto-acoustic imaging is its impressive spatial resolution and tissue penetration capabilities, which go beyond the limits of traditional optical imaging:
- Deep Tissue Penetration: Unlike standard optical imaging, which struggles with light scattering in tissues, opto-acoustic imaging penetrates several centimeters into tissue while maintaining high resolution.
- High Contrast Imaging: The combination of deep penetration from ultrasound and the high contrast provided by optical imaging ensures that both superficial and deep tissues are clearly visualized, making it an especially effective tool for breast imaging.
Why This Matters for Breast Imaging
In breast imaging, the ability to detect deep-seated structures is essential, especially in patients with dense breast tissue that can obscure abnormalities in traditional imaging. Opto-acoustic imaging provides high-resolution, dynamic images that show not just the structure but also how blood flow and oxygenation patterns change in real-time, giving a clearer view of potential tumors.
This makes opto-acoustic imaging a valuable tool in the early detection of breast cancer, potentially reducing the need for invasive procedures like biopsies. By offering both anatomical and functional perspectives, this technology enhances diagnostic accuracy and improves patient outcomes.
Summary: The Future of Breast Imaging
Opto-acoustic imaging combines the strengths of optical and ultrasound technologies to create detailed, real-time images of breast tissue. Its ability to visualize deep tissues with high resolution and capture dynamic changes in blood flow and oxygenation makes it a promising tool for early breast cancer detection. This innovation could reduce the need for invasive procedures and ultimately improve patient care.
How Opto-Acoustic Imaging Leverages Tissue Properties for Enhanced Breast Imaging
“Opto-acoustic imaging offers a unique approach by differentiating tissues based on how they absorb infrared light and emit sound waves.”
Tissue Absorption and Sound Wave Generation
At the core of opto-acoustic breast imaging is the ability to distinguish tissues based on their absorption of infrared light and the corresponding sound waves they generate. As tissues absorb infrared light, they produce sound waves that vary in intensity and frequency. These sound wave patterns provide detailed insights into the tissue’s density, composition, and health.
- Infrared Light Absorption: Different tissues absorb light at varying degrees, depending on factors like density and composition.
- Sound Wave Emission: Once absorbed, tissues emit sound waves that can be measured and analyzed for their distinct characteristics, forming the basis of opto-acoustic imaging.
Functional Differences Between Healthy and Diseased Tissues
Opto-acoustic imaging goes beyond visualizing tissue structure; it captures functional differences that are often more telling in diagnosing conditions like cancer. Diseased tissues, particularly tumors, exhibit altered metabolic rates, increased oxygen consumption, and abnormal vascularization. These functional differences create unique optical and acoustic signatures, which can be captured by opto-acoustic technology.
Key Biological Indicators in Cancer Detection
Some of the most important indicators of tissue health that opto-acoustic imaging can detect include:
- Hemoglobin Concentration: Cancerous tissues often have altered hemoglobin levels due to abnormal blood supply.
- Oxygen Uptake and Hypoxia: Tumors frequently display hypoxia, a condition characterized by low oxygen levels resulting from rapid growth and inefficient vascularization. These areas of low oxygen are easily identified using opto-acoustic techniques, providing crucial insights into tumor behavior.
- Metabolic Rates: Tumor tissues typically have higher metabolic activity than normal tissues, which leads to changes in light absorption and sound wave patterns.
Real-Time Insights for Improved Diagnostics with Opto-Acoustic Imaging
Advantages Over Traditional Breast Imaging Methods
“Opto-acoustic imaging provides real-time functional data, enhancing diagnostic accuracy by offering deeper insights into tissue health compared to conventional methods.”
Opto-acoustic imaging delivers significant benefits over traditional breast imaging techniques like mammography and ultrasound. While conventional methods typically focus on identifying structural changes in the tissue, opto-acoustic technology allows clinicians to examine functional differences such as metabolic activity and vascular patterns. These functional insights give a more comprehensive view of tissue health, helping to identify potential malignancies with greater precision.
Key Functional Parameters for Enhanced Diagnosis
The real-time data captured by opto-acoustic imaging focuses on several critical functional parameters, including:
- Tissue Oxygenation: Opto-acoustic imaging can reveal differences in oxygen levels between healthy and cancerous tissue, providing an early indication of malignancy.
- Blood Flow Patterns: The technology helps visualize abnormal blood flow that often accompanies tumor growth, aiding in the early detection of aggressive cancers.
- Vascular State: By detecting abnormal vascular networks, opto-acoustic imaging can highlight areas of concern that might otherwise be missed in standard imaging.
Reducing the Need for Invasive Procedures
One of the most significant advantages of opto-acoustic imaging is its potential to reduce the need for invasive procedures like biopsies. Traditional imaging techniques can sometimes produce inconclusive results, leading to unnecessary biopsies that carry risks of complications and patient anxiety. Opto-acoustic imaging, by providing more detailed and functional data, can help clinicians make more informed decisions without resorting to invasive diagnostics.
A Powerful Tool in the Fight Against Breast Cancer
By integrating these functional insights with high-resolution imaging, opto-acoustic technology enhances the accuracy of breast cancer diagnosis. This is particularly useful in challenging cases where conventional imaging does not provide definitive results. With its ability to differentiate between benign and malignant lesions based on tissue function, opto-acoustic imaging is proving to be a critical tool in advancing breast cancer care.
Enhancing Breast Cancer Detection with Opto-Acoustic Imaging
How Opto-Acoustic Imaging Works
Opto-acoustic imaging leverages the differential absorption of infrared light to not only capture anatomical details but also provide real-time data on the functional characteristics of breast tissue. By observing the tissue’s metabolic activity, oxygen consumption, and blood flow patterns, clinicians can distinguish between healthy and diseased areas more accurately.
“Unlike traditional ultrasound, which identifies masses, opto-acoustic imaging offers a comprehensive view of both the structural and metabolic states of breast tissues.”
The Role of Functional Data in Identifying Suspicious Lesions
Standard imaging techniques like ultrasound can detect the presence of a mass, but they often fail to provide the functional information needed to differentiate between benign and malignant lesions. Opto-acoustic imaging fills this gap by delivering critical insights into tissue health:
- Metabolic Activity: Abnormal tissue growths, such as tumors, have higher metabolic rates and oxygen consumption, which are visible in opto-acoustic scans.
- Blood Flow Patterns: The imaging technique can directly observe abnormal blood vessel growth (angiogenesis), a common indicator of cancerous tissues.
By analyzing these parameters, opto-acoustic imaging enhances the accuracy of breast cancer detection, particularly in early stages when treatment is most effective.
Distinguishing Between Benign and Malignant Tumors
Studies have shown that tumors absorb infrared light differently from normal tissues due to their abnormal vascular networks and higher metabolic demands. This creates distinct acoustic signals that clinicians can use to map oxygenated and deoxygenated blood levels within breast tissues. These signals provide critical information about the tissue’s health, helping doctors identify malignant growths earlier and more accurately than with traditional imaging alone.
Contrast-Free Imaging for Safer Diagnostics
One of the major benefits of opto-acoustic imaging is its ability to assess tissue health without the need for contrast agents, which are commonly used in MRI or CT scans. Contrast agents, while useful, carry risks for patients with kidney issues or allergies. Opto-acoustic imaging avoids these risks by relying on the natural absorption of light by the tissue. However, for cases requiring enhanced imaging, opto-acoustic techniques can still be combined with targeted contrast agents to improve diagnostic accuracy.
A Revolution in Breast Cancer Diagnostics
As research progresses, opto-acoustic imaging is proving to be a game-changer in breast cancer diagnostics. Its ability to visualize both the structure and function of breast tissues in real time allows for more informed decisions in patient care. This technology:
- Reduces the need for invasive biopsies by providing non-invasive assessments of tissue health.
- Improves the specificity of breast cancer screening, leading to earlier detection.
- Enhances patient outcomes by offering clinicians deeper insights into tissue behavior and tumor growth.
To dive deeper into the metabolic differences between healthy and diseased tissues, and how imaging technologies detect these differences, explore this comprehensive study or read this research on tumor metabolism and imaging.
How Opto-Acoustic Imaging Detects Cancer through Blood Oxygenation and Hemoglobin Mapping
1. Unique Metabolic Profile of Cancerous Tissues
Cancerous tissues have a distinct metabolic profile, particularly in their rapid consumption of oxygen. Compared to healthy tissues, cancer cells deplete blood oxygen more quickly, leading to hypoxic (low-oxygen) regions within tumors. These hypoxic areas can be distinctly visualized with opto-acoustic imaging, as they contrast sharply with surrounding oxygen-rich tissues. This technique capitalizes on these oxygen differences, creating detailed, color-coded maps of oxygenated and deoxygenated blood, as well as hemoglobin concentration. These maps are crucial for precisely localizing cancerous masses and distinguishing them from benign tissues.
“By creating color-coded maps of blood oxygen levels, opto-acoustic imaging provides a more accurate method of identifying cancerous tissues.”
2. Laser Wavelengths and Hemoglobin Absorption
Opto-acoustic imaging relies on the selective absorption of laser light at specific wavelengths to differentiate between oxygenated and deoxygenated blood. Typically, the wavelengths used fall within the near-infrared (NIR) spectrum. Here’s why:
- Oxygenated Hemoglobin: Absorbs more light at certain NIR wavelengths.
- Deoxygenated Hemoglobin: Absorbs more light at different NIR wavelengths.
By using lasers tuned to these specific wavelengths, opto-acoustic imaging can target and visualize blood oxygenation levels within tissues. This is particularly useful for identifying cancerous tissues, which often exhibit abnormal blood flow and oxygenation patterns due to their high metabolic demands and inefficient vascular networks.
Learn more about how hemoglobin mapping aids in cancer detection.
3. Benefits of Opto-Acoustic Imaging Over Traditional Modalities
One of the most significant advantages of opto-acoustic imaging is its ability to differentiate tissue types without the need for exogenous contrast agents. Traditional imaging modalities, such as CT or MRI, often require contrast agents to highlight differences between healthy and diseased tissues. However, these agents can pose risks, particularly for patients with kidney issues or allergies. Opto-acoustic imaging offers a safer alternative by utilizing the body’s natural chromophores, like hemoglobin, to generate high-contrast images. This non-invasive approach reduces patient risk while still providing highly detailed functional and anatomical information.
- Non-Invasive: No contrast agents needed.
- Safe for High-Risk Patients: Ideal for those with allergies or kidney conditions.
- Highly Detailed Imaging: Provides both functional and structural insights.
Read more about the safety benefits of non-invasive imaging techniques.
Opto-acoustic imaging bypasses the need for invasive procedures, offering a revolutionary approach to cancer detection through blood oxygenation and hemoglobin mapping.
The Power of Combining Opto-Acoustic Imaging with Ultrasound
Integrating opto-acoustic imaging with conventional ultrasound creates a robust dual-modality system that significantly enhances diagnostic accuracy. While conventional ultrasound excels in providing detailed anatomical images, it lacks the capability to assess the metabolic activity or oxygenation levels of tissues. Opto-acoustic imaging fills this gap by offering functional insights, giving clinicians a comprehensive view of the breast’s structure and function.
Advantages of Dual-Modality Approach
- Comprehensive Tissue Analysis: Ultrasound captures detailed anatomical information, while opto-acoustic imaging reveals the metabolic activity and oxygenation status of tissues.
- Enhanced Angiogenesis Detection: Tumors often stimulate the growth of new blood vessels (angiogenesis) to support their rapid growth. These vessels tend to be disorganized and inefficient, leading to areas of deoxygenated blood, which can be easily detected with opto-acoustic imaging.
“By combining anatomical detail from ultrasound with functional insights from opto-acoustic imaging, clinicians gain a fuller understanding of breast tissue, improving the detection and assessment of malignancies.”
Angiogenesis as an Indicator of Malignancy
Opto-acoustic imaging plays a key role in mapping regions of angiogenesis and identifying areas with a high concentration of deoxygenated blood. This information is crucial in distinguishing between benign and malignant breast lesions. Tumors often induce angiogenesis, leading to poorly organized, inefficient blood vessels, which result in increased areas of deoxygenated blood. Opto-acoustic imaging captures these details, providing radiologists with critical insights.
- Angiogenesis Mapping: Helps identify poorly organized blood vessels associated with tumor growth.
- Deoxygenated Blood Detection: Pinpoints areas of low oxygen, which are common in malignant tumors.
Early Detection and Monitoring with Opto-Acoustic Imaging
One of the standout features of opto-acoustic imaging is its ability to detect early signs of malignancy by identifying angiogenesis and deoxygenated blood. For example, a breast lesion with significant angiogenesis and high levels of deoxygenated blood is more likely to be malignant. By recognizing these key indicators, opto-acoustic imaging improves early breast cancer detection, allowing for timely diagnosis and treatment.
This technology is also highly suited for repeated use because it does not rely on invasive procedures or contrast agents. This makes opto-acoustic imaging an ideal tool for monitoring tumor progression and evaluating a patient’s response to therapy over time.
Improving Personalized Breast Cancer Care
Overall, the integration of opto-acoustic imaging with ultrasound represents a significant advancement in breast cancer diagnostics. Its real-time, high-resolution images of both anatomical and functional tissue characteristics offer a more nuanced and accurate assessment of potential malignancies. As research continues to validate its effectiveness, opto-acoustic imaging is expected to become a vital component of personalized breast cancer care, ultimately improving patient outcomes through more precise clinical decision-making.
Discover more advancements in radiologic technologies that are shaping the future of breast cancer diagnosis and treatment.
About the Procedure: How Opto-Acoustic Imaging Works in Practice
Opto-acoustic imaging is an advanced diagnostic technique that merges laser technology with the capabilities of ultrasound to provide a comprehensive view of breast tissue. The process is non-invasive, using specific wavelengths of light to generate acoustic signals that reveal both anatomical and functional information about the tissue. Here’s how it works step by step:
1. Laser Light Penetration
- Near-infrared light, typically between 550 nm and 900 nm, is directed at the breast tissue where a potential malignancy is suspected.
- These wavelengths are chosen because they deeply penetrate breast tissue while being absorbed by biological molecules, such as hemoglobin, which are present in higher concentrations in cancerous tissues.
2. Differential Absorption and Tissue Heating
As the light penetrates the breast, cancerous tissues absorb more light than healthy tissues due to their elevated metabolic rates and increased hemoglobin levels. This higher absorption causes a minor thermal expansion, generating sound waves within the tissue.
“The interaction of laser light with breast tissue causes minimal heating, producing sound waves that travel through the tissue, offering vital clues about blood oxygenation and hemoglobin concentration.”
3. Sound Wave Detection
The slight expansion from tissue heating creates broadband, low-amplitude sound waves. These pressure waves are captured by a sensor array in the transducer head placed over the breast. The sensor array detects the weak acoustic signals with high sensitivity, converting them into electrical signals.
4. Image Reconstruction
- The electrical signals from the transducer are sent to a computer where advanced algorithms reconstruct detailed 2D images of the breast.
- These images highlight differences in tissue composition, with cancerous tissues standing out due to their higher light absorption and stronger acoustic signals.
Learn more about how light absorption by chromophores aids in cancer detection.
Advantages of Opto-Acoustic Imaging
One of the significant benefits of opto-acoustic imaging is its ability to provide real-time, non-invasive imaging without the use of contrast agents or invasive procedures. Key functional metrics, such as:
- Blood Oxygenation Levels
- Hemoglobin Concentration
- Tissue Metabolism
These metrics are critical for diagnosing breast cancer and are made visible through opto-acoustic technology. The real-time nature of this imaging allows healthcare providers to make informed decisions about the need for further diagnostic steps or treatment options on the spot.
Dual-Modality Approach: Combining Ultrasound and Opto-Acoustic Imaging
Opto-acoustic imaging integrates seamlessly with traditional ultrasound, combining structural and functional insights in one comprehensive scan:
- Ultrasound: Offers high-resolution anatomical details.
- Opto-Acoustic Imaging: Adds functional data such as blood flow and oxygenation.
“This dual-modality approach enhances diagnostic accuracy, especially in complex cases where the distinction between benign and malignant tissues is unclear.”
Early Detection and Reduced Need for Biopsies
One of the most promising applications of opto-acoustic imaging is in early breast cancer detection. By non-invasively identifying the functional characteristics of tissue, it reduces the likelihood of unnecessary biopsies. In addition, it helps guide treatment planning by providing real-time insights into tissue health.
- Non-invasive: No need for contrast agents or invasive biopsies.
- Personalized Care: The technique supports more accurate and timely patient care, enhancing overall diagnostic precision.
For more on the benefits of opto-acoustic imaging in cancer detection, check out this research on tumor metabolism and imaging.
Advanced Image Reconstruction and Contrast in Opto-Acoustic Imaging
Opto-acoustic imaging, also known as photo-acoustic imaging, offers a major leap forward over conventional ultrasound (US), providing superior tissue differentiation and imaging specificity. This innovative technique combines light absorption and sound wave generation within tissues to produce detailed, high-resolution images. Here’s how the advanced image reconstruction and contrast work in opto-acoustic imaging:
Image Reconstruction: A Key Difference from Ultrasound
One of the critical aspects of opto-acoustic imaging is the image reconstruction process. Like ultrasound, it uses the time delay of acoustic waves reaching the sensors to construct an image. However, the approach differs significantly in how the beams are focused.
- Conventional Ultrasound: Both the transmit and receive beams are focused, allowing precise localization of tissues.
- Opto-Acoustic Imaging: The transmit beam (laser light) scatters in tissues with varying densities, especially beyond 1 millimeter. Therefore, only the receive beam (sound waves) is focused to create the final image.
“In opto-acoustic imaging, the laser light scatters as it passes through tissues, but the sound waves are collected and focused, creating high-resolution images.”
This focusing of sound waves allows for the collection of detailed acoustic signals, which are processed through advanced algorithms to reconstruct highly accurate, high-contrast images.
Absorption-Based Contrast: A Unique Advantage
In conventional ultrasound, contrast is generated based on the mechanical and elastic properties of tissues—essentially how much the tissues resist the passage of sound waves. This can make it difficult to differentiate between tissues with similar acoustic properties.
Opto-acoustic imaging, on the other hand, creates images based on optical absorption properties:
- Images are formed based on the amount of light energy absorbed and converted into sound waves by the tissues.
- The initial pressure distribution, generated by the absorption of light energy, forms the basis for image contrast.
- Different tissues absorb light at different rates, depending on their composition—such as the presence of hemoglobin, water, or lipids.
This absorption-based contrast provides much greater tissue specificity. For example, hemoglobin, abundant in blood, strongly absorbs light, making opto-acoustic imaging particularly effective in visualizing microvasculature—tiny blood vessels that are often invisible in traditional ultrasound due to weak echogenicity.
Visualizing Blood Flow and Oxygenation
The enhanced contrast capability of opto-acoustic imaging is invaluable for visualizing biological structures, particularly those related to blood flow and tissue oxygenation:
- It enables the detection of microvasculature, which is critical for diagnosing conditions like cancer.
- The ability to visualize tissue oxygenation provides key insights, especially in detecting tumors, where abnormal blood vessel growth (angiogenesis) is a hallmark of development.
“Opto-acoustic imaging’s ability to clearly map blood vessels and tissue oxygenation offers critical insights into tumor development and other conditions.”
For instance, cancerous tissues typically exhibit abnormal vascularization, and the ability to see these small vessels in detail can significantly aid early detection.
Applications in Oncology and Beyond
The precision of opto-acoustic imaging makes it particularly useful in fields where detailed visualization of blood vessels and tissue oxygenation is essential:
- Oncology: Detecting tumors by observing abnormal blood vessel growth and oxygenation patterns.
- Cardiology: Assessing blood flow and detecting atherosclerotic plaques.
- Vascular Imaging: Providing detailed insights into the microvasculature for better diagnosis and treatment planning.
Overall, opto-acoustic imaging’s ability to generate high-resolution, absorption-based contrast images makes it a superior tool for applications requiring precise tissue differentiation and vascular visualization. Its reliance on optical properties rather than acoustic impedance sets it apart from traditional imaging techniques, offering enhanced diagnostic capabilities across a wide range of medical fields.
To explore more on how opto-acoustic imaging enhances cancer diagnostics, visit this study on tumor hypoxia and optical imaging.
Pros and Cons of Opto-Acoustic Imaging Compared to Other Breast Cancer Diagnostic Tools
Breast cancer diagnosis involves multiple imaging techniques, each with distinct strengths and limitations. Common methods include blood marker tests, breast MRI, CT scans, PET scans, chest X-rays, mammograms, and ultrasounds. Among these, mammograms and ultrasounds are most frequently used. However, they present certain drawbacks that highlight the potential benefits of opto-acoustic imaging as a complementary or alternative diagnostic tool.
Mammograms
- Strengths: Mammograms are considered the gold standard for breast cancer screening, especially in older women. They are effective at detecting calcifications and early-stage tumors.
- Limitations:
- The procedure can be uncomfortable or painful due to the compression of breast tissue.
- It is time-consuming, taking about 20 minutes per breast.
- Less effective in younger women with dense breast tissue, leading to false-negative results where tumors might go undetected.
- Dense tissue may also lead to false-positive results, causing unnecessary anxiety and additional testing.
Ultrasound
- Strengths: Ultrasound is non-invasive, uses no ionizing radiation, and is effective at distinguishing between solid masses and fluid-filled cysts. It is often used to further investigate abnormalities found in mammograms.
- Limitations:
- While it can detect the presence of a mass, ultrasound cannot determine whether the mass is malignant or benign, often requiring biopsies for confirmation.
- Ultrasound struggles to visualize very small or deep-seated tumors, which can result in incomplete assessments.
Opto-Acoustic Imaging
Opto-acoustic imaging offers distinct advantages, addressing several of the limitations of mammograms and ultrasounds:
-
- Combination of Ultrasound and Light Absorption: Opto-acoustic imaging combines high-resolution ultrasound with functional imaging based on light absorption. It provides detailed images focused on hemoglobin content and blood oxygenation levels, which are key indicators of abnormal tissue growth.
- Microvasculature Visualization: A major benefit is its ability to visualize the microvasculature—tiny blood vessels crucial for assessing tumor growth. This is particularly helpful for:
- Detecting tumors in younger women with dense breast tissue where mammograms are less effective.
- Highlighting vascular changes that might not be fully captured by ultrasound.
- Non-Invasive and Radiation-Free: Opto-acoustic imaging doesn’t use ionizing radiation, making it a safer option for repeated screenings or for patients sensitive to radiation.
“Opto-acoustic imaging provides a safer, non-invasive alternative for breast cancer screening, offering both anatomical and functional insights, especially in dense breast tissue.”
- Limitations:
- As a relatively new technology, opto-acoustic imaging is still primarily available in research settings and specialized clinics, limiting its accessibility.
- It requires sophisticated equipment and trained personnel, which may increase costs.
- Best used in conjunction with other imaging modalities for a comprehensive diagnosis.
Conclusion
While traditional diagnostic tools like mammograms and ultrasounds are essential for breast cancer detection, they have limitations that opto-acoustic imaging can address. Opto-acoustic imaging offers a non-invasive, radiation-free alternative, providing both structural and functional information about breast tissues. This technology excels in difficult cases involving dense breast tissue and the need for precise vascular imaging. As it becomes more widely available, opto-acoustic imaging holds great promise for enhancing breast cancer detection and diagnosis, ultimately improving patient outcomes.
Advantages of Opto-Acoustic Breast Imaging Technique
Opto-acoustic breast imaging offers a variety of advantages, effectively addressing many limitations found in traditional breast cancer diagnostic methods. As a non-invasive, cost-effective, and easy-to-administer technique, it provides an appealing alternative for both patients and healthcare providers.
Non-Invasive and Safer for Patients
- No Ionizing Radiation: Unlike other imaging methods, opto-acoustic imaging does not rely on ionizing radiation, making it a safer option for both the patient and the technician.
- No Contrast Agents: This technique eliminates the need for contrast agents or dyes, which are commonly used in other imaging modalities like MRI. This is particularly beneficial for patients with allergies or kidney issues, who may be at risk from these agents.
- Comfortable Procedure: The procedure is quick and does not involve the painful breast compression typically required for mammograms. Patients remain comfortably lying down while the sensor array is placed over the area of interest, greatly reducing discomfort and anxiety.
High Sensitivity and Specificity
“Opto-acoustic imaging combines the precision of light-based imaging with the sensitivity of ultrasound, providing high-resolution images that can detect tumors as small as 2 mm.”
One of the key strengths of opto-acoustic imaging is its ability to provide high sensitivity and specificity, which is essential for accurate diagnosis. Ongoing clinical trials have shown that opto-acoustic imaging can detect tumors as small as 2 mm, potentially even smaller. Early detection of such highly malignant tumors increases the chances of successful treatment, making this capability crucial in improving patient outcomes.
Accurate Differentiation of Malignant and Benign Lesions
- Detailed Imaging: The high-resolution images produced by opto-acoustic imaging allow radiologists to analyze the mass and surrounding tissues in great detail, providing vital information about the lesion’s nature.
- Enhanced Diagnostic Accuracy: When combined with traditional ultrasound, which excels in identifying the shape and size of a lesion, opto-acoustic imaging provides a comprehensive view that improves diagnostic accuracy.
- Deep Tissue Penetration: The deep penetration of laser light allows for a more thorough examination of the lesion’s location and extent, giving radiologists a clearer and more precise diagnostic picture.
Ideal for Younger Women and Dense Breast Tissue
Traditional mammography often struggles with younger women due to their dense breast tissue, active milk glands, and higher proportions of glandular tissue, which can obscure tumors and lead to false positives or negatives. Opto-acoustic imaging, however, is not affected by breast tissue density, making it an effective tool for women of all ages. This technology significantly reduces the chances of misdiagnosis by providing reliable results across diverse patient populations.
Conclusion
Opto-acoustic breast imaging represents a significant advancement in breast cancer diagnostics. Its non-invasive nature, high sensitivity, and ability to differentiate between malignant and benign lesions make it a highly valuable tool. Additionally, the technique’s efficacy in dense breast tissue makes it especially useful for younger women. By offering a safer and more comfortable alternative to traditional imaging, opto-acoustic imaging has the potential to improve early detection, enhance diagnostic accuracy, and ultimately, contribute to better patient outcomes.
Reducing Unnecessary Biopsies with Opto-Acoustic Imaging
One of the most promising aspects of opto-acoustic imaging is its ability to reduce the number of unnecessary biopsies. Clinical trials are showing that this advanced technique can effectively distinguish between benign and malignant breast lumps. For patients with benign lumps, this means they can avoid invasive biopsies, sparing them from the anxiety, discomfort, and potential complications that come with these procedures.
“By clearly identifying benign lumps, opto-acoustic imaging not only enhances patient comfort but also cuts down on the overall costs associated with breast cancer diagnostics.”
- Less Invasive: Opto-acoustic imaging reduces the need for unnecessary biopsies by providing accurate, non-invasive results.
- Cost-Effective: By avoiding unnecessary procedures, this technology helps reduce healthcare costs associated with breast cancer diagnostics.
- Improved Patient Experience: Patients benefit from less anxiety and discomfort, as fewer biopsies are needed.
Personalized Cancer Care
Researchers are also investigating how opto-acoustic imaging results correlate with cancer stages identified through laboratory analysis. By understanding this correlation, opto-acoustic imaging could become a crucial tool in personalized cancer care. The ability to tailor treatment plans based on the stage of cancer detected through this imaging technique would provide a more targeted approach to breast cancer treatment.
With the potential to offer real-time insights into tumor growth, blood oxygenation, and metabolic activity, opto-acoustic imaging could help oncologists design more effective treatment strategies that are customized to the patient’s specific condition. This personalized approach could lead to improved outcomes, particularly when combined with other advanced diagnostic techniques.
Why Opto-Acoustic Imaging Is a Game Changer
Opto-acoustic breast imaging stands out from traditional diagnostic methods for several reasons:
- Non-Invasive and Comfortable: Unlike mammograms, this technique does not involve painful breast compression, and it is radiation-free, making it a safer and more patient-friendly option.
- High Sensitivity and Specificity: The high-resolution images provided by opto-acoustic imaging allow for early detection of breast cancer, including differentiating between benign and malignant lumps with remarkable accuracy.
- No Need for Contrast Agents: Unlike other imaging techniques that require contrast agents, opto-acoustic imaging uses the body’s natural light absorption properties, reducing the risk for patients, particularly those with allergies or kidney issues.
- Personalized Care: As research evolves, opto-acoustic imaging is expected to play a pivotal role in personalized cancer care by offering deeper insights into tumor characteristics and progression.
The Future of Breast Cancer Diagnostics
As clinical trials continue to validate the effectiveness of opto-acoustic imaging, this technology is poised to become an integral part of breast cancer diagnostics. Its ability to provide detailed, high-resolution images without the need for ionizing radiation or contrast agents makes it a safer, more comfortable option for patients. Additionally, the technique’s specificity in distinguishing between benign and malignant lesions has the potential to reduce the number of unnecessary biopsies.
In summary, opto-acoustic imaging offers a unique combination of safety, comfort, and diagnostic accuracy, which could revolutionize the early detection and treatment of breast cancer. With ongoing research and further clinical validation, it is likely to become a key player in improving patient outcomes through more accurate and personalized care. For more information about this technology, visit Mammography Resources.
References
- http://www.medgadget.com/2014/04/seno-imagio-opto-acoustic-breast-cancer-imaging-system-cleared-in-europe.html
- http://consultqd.clevelandclinic.org/2014/06/opto-acoustic-breast-imaging-can-it-reduce-the-need-for-breast-biopsy/
- http://www.medscape.com/viewarticle/780708_6
- senomedical.com
- http://www.breastcancer.org/symptoms/testing/types/ultrasound
- http://medicalphysicsweb.org/cws/article/newsfeed/55693
- http://rsfs.royalsocietypublishing.org/content/royfocus/1/4/602.full.pdf
Here is details about continuing education credits for radiologic technologists.
FAQs
1. What is opto-acoustic breast imaging, and how does it work?
Opto-acoustic breast imaging is a hybrid imaging technique that combines laser optics and ultrasound to create detailed images of breast tissue. It works by using laser pulses to irradiate the tissue, causing a small rise in temperature that generates ultrasound waves. These waves are then captured and processed to create high-resolution images, providing valuable information about the tissue’s structure and composition.
2. What are the advantages of opto-acoustic breast imaging over traditional imaging methods?
Opto-acoustic breast imaging offers several advantages over traditional imaging methods, such as mammography and ultrasound. It provides better contrast in visualizing blood vessels and tissue oxygenation, making it particularly useful in detecting tumors that are difficult to see with other methods. Additionally, it does not involve ionizing radiation, making it a safer option for patients.
3. How does opto-acoustic imaging enhance the detection of breast cancer?
Opto-acoustic imaging enhances breast cancer detection by providing detailed information about the vascular structure and oxygenation of breast tissue. Tumors often have increased blood vessel formation and different oxygenation levels compared to normal tissue, which opto-acoustic imaging can detect with high sensitivity. This allows for earlier and more accurate identification of malignant lesions.
4. Is opto-acoustic breast imaging safe for repeated use, and does it involve any risks?
Yes, opto-acoustic breast imaging is safe for repeated use as it does not involve ionizing radiation, unlike mammography. The technique uses laser light and ultrasound, both of which are non-invasive and pose minimal risk to patients. This makes it suitable for frequent monitoring of breast health, especially in high-risk individuals.
5. How does opto-acoustic imaging compare to other advanced breast imaging techniques like MRI and 3D ultrasound?
Opto-acoustic imaging complements other advanced breast imaging techniques like MRI and 3D ultrasound by providing additional information about tissue vascularity and oxygenation that these methods may not fully capture. While MRI offers excellent soft tissue contrast and 3D ultrasound provides detailed anatomical information, opto-acoustic imaging adds functional data that can enhance the overall assessment of breast lesions. It is especially useful when combined with other modalities for a more comprehensive evaluation.
