DXA Scanning in Clinical Practice: An Overview for X-ray Techs
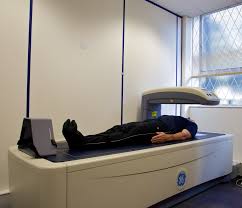
DXA is a noninvasive modality used to measure bone density. It is also known as bone density scanning, bone densitometry, and BMD testing. This overview of DXA scanning in clinical practice will allow DXA operators and other radiologic technologists to review and refresh their knowledge about this imaging modality.
DXA scanning in clinical practice creates a planar 2D image. It does not take into account bone depth. Bone density by DXA is thus reported in grams/square centimeters. Lack of representation of the body as a true 3D structure is the primary limitation of DXA. Nonetheless, at the current time, DXA scanning in clinical practice is the method of choice to measure BMD and diagnose bone diseases such as osteoporosis. This is because it is an optimal combination of cost effectiveness, accuracy, and availability. There are an estimated 50,000 DXA systems in use around the world.
What Information Does a DXA Scan Provide?
BMD measurement by DXA scanning in clinical practice is an indicator of bone strength and fracture risk. There is a roughly 1.6-times increment in fracture risk for a single standard deviation decrement in bone mineral density. Results from a DXA scan are compared to reference populations defined by age, gender, and ethnicity. Therefore, an individual’s DXA result is compared to a young healthy population or to a peer group.
DXA is also used to monitor the effects of osteoporosis therapy and to track changes in other medical conditions associated with bone loss. DXA measures bone density at central as well as axial sites (spine and hip, respectively). It can, in addition, be used to calculate bone density at the forearm or the total body.
Limitations of DXA
Extensive epidemiological data is available about DXA. This method of BMD measurement has been validated by a number of clinical trials. However, as mentioned, one major disadvantage of DXA scanning in clinical practice is that it measures BMD in grams/cm2 (area). Therefore, the depth of the tissue is not accounted for. Also, this modality does not differentiate between the two types of bone (cortical and trabecular). This makes measurements likely to be an over-estimation of bone density.
Sites of DXA Scanning
DXA scanning in clinical practice is performed at well-defined skeletal sites, including the lumbar spine, hip, and forearm. In a standard scan, the hip and spine are imaged. If one of these sites is unavailable, the forearm is included.
DXA Technology
DXA is essentially the X-ray equivalent of DPA. DXA uses X-ray technology and exposes the patient to a small amount of ionizing radiation. X-ray technologists are exposed to very little scatter radiation when performing DXA scanning in clinical practice. Absorptiometry measures the attenuation (reduction in intensity) of X-ray beams caused by body tissues. Denser tissues cause more reduction in intensity of the beam.
DXA is superior to SXA because DXA utilizes an extra X-ray beam with a different attenuation profile. The two beams are aimed at the patient’s body and are absorbed differently by bone and soft tissue. The additional beam in DXA is used to calculate the attenuation caused by soft tissues and subtract it from the attenuation caused by bone for more accurate BMD results.
Fracture Detection with DXA
In addition to bone density, fan-beam DXA scanning in clinical practice is used to obtain images of the spine with moderate resolution. These lateral thoracic and lumbar images are helpful in identifying moderate to severe fractures in the vertebrae with more than 90 percent specificity and sensitivity. It should be noted that DXA imaging has limited use in identifying mild fractures of the vertebrae. DXA-based vertebral fracture assessment (VFA) is especially useful in clinical settings when, if present, one or more fractures in the vertebrae would alter the patient’s management.
DXA Manufacturers
Machines for DXA scanning in clinical practice have been commercially available since 1987. The major manufacturers of DXA equipment in the United States are Hologic, Norland, and GE-Lunar. There are more than 10,000 DXA machines in America. The reliability and precision of DXA machines, both in the short- and long-term, has been proven by many studies. At the present time, DXA is the most frequently used and most widely available modality for bone mineral density measurement. DXA scans are also useful in body composition analysis and calculating the fat content of the body. DXA scanners are therefore used in clinical research and to evaluate adiposity in children.
DXA versus FRAX
It is worth noting that despite cohort studies indicating that DXA scanning in clinical practice is predictive of fracture risk, this epidemiological evidence is not always applicable to the individual patient in the clinical setting. The World Health Organization’s FRAX tool released in 2009 is a better predictor of a patient’s fracture risk because it takes into account BMD measurement by DXA as well as other risk factors including gender, age, and previous fragility fractures.
It should be noted, however, that FRAX scores do not typically affect clinical management in patients who have an established diagnosis of osteoporosis or patients with normal BMD. FRAX is mainly useful in the management of patients with osteopenia (low bone mass).
Continuing Education for X-ray Technologists
We offer online CE courses for X-ray technologists to complete ARRT® requirements. To purchase X-ray continuing education e-courses, please visit our shop and choose the type and number of credits you need. Our bone densitometry course is appropriate for both DXA operators and general radiographers. It is worth 23 CEUs and is an easy way to complete the bulk of your biannual CE requirements.
Visit here for more information about California fluoroscopy ce credits.