Bone Disease Medical Treatment: A Brief Guide for DXA Technologists
There are specific bone disease medical treatments available for a number of diseases (other than osteoporosis). These include congenital disorders and bone problems associated with kidney disease. These treatments are effective, safe, and often curative. Early recognition and therapy for these conditions is critical. They include rickets, osteomalacia, and hyperparathyroidism. Early treatment can help avoid fractures, crippling deformities, and chronic complications.
Primary Hyperparathyroidism
This condition is caused by an excessive secretion of PTH from the parathyroid glands. Is there a bone disease medical treatment for this condition? The definitive treatment for primary hyperparathyroidism is surgical. This is recommended if the cause of excessive PTH release is determined to be a benign parathyroid tumor (adenoma). Surgical removal of three and a half enlarged glands (leaving half a gland intact) is often curative. The NIH has concluded that patients with clear symptoms, such as kidney stones or bone disease, are good candidates for parathyroidectomy surgery.
What is the best course of action in patients who are asymptomatic? Is there a need for intervention in patients with no clear signs or symptoms of primary hyperparathyroidism? The bone disease medical treatment in this instance is controversial. Guidelines suggest that treatment should be given to patients who are less than 50 years old. Also, patients who have hypercalcemia with calcium levels more than 1 mg/dL above the upper limit of normal are candidates for treatment. In addition, hypercalciuria with more than 400 mg of urinary calcium excretion is an indication for treatment. According to an NIH panel of experts, however, asymptomatic patients with primary hyperparathyroidism should be treated based on their bone density. This should be according to the established definition of osteoporosis. Thus, surgery is recommended in patients with a T-score of -2.5 or less at any skeletal site.
Effectiveness of Surgery for Primary Hyperparathyroidism
Instead of bone disease medical treatment, evidence suggests that surgery for primary hyperparathyroidism is an effective treatment. Following parathyroidectomy, patients gain at least 10 percent bone mass in the ensuing 3-4 years. The largest improvement is noted in the spine. Studies have also found that patients who are status post parathyroidectomy surgery have a reduced rate of fractures.
Parathyroid Surgery
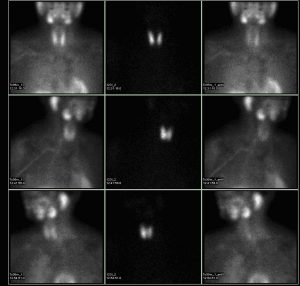
Removal of the glands is a complex procedure that requires exceptional skill and expertise. The enlarged glands must be carefully identified and removed without injuring surrounding tissues. Advances in surgical technique have led to newer approaches. These include minimally invasive surgery which requires only a small incision. A single parathyroid adenoma is removed with very little trauma to surrounding tissue. Before minimally invasive surgery can be performed, however, the location of the abnormal parathyroid gland needs to be identified. This is done with the help of a Sestamibi scan using technicium-99m or with ultrasound imaging. Patients who are not good candidates for parathyroid surgery can be managed effectively with more conservative measures. Bone disease medical treatment includes avoiding dehydration and preventing further bone loss.
Medical Treatment for Primary Hyperparathyroidism
Calcimimetic drugs like Sensipar (cinacalcet hydrochloride) mimic the action of calcium and bring down high levels of PTH. They are therefore a good bone disease medical treatment for this condition. However, currently the U.S. Food and Drug Administration has not approved these medications for primary hyperparathyroidism. Sensipar is approved for the treatment of patients with chronic kidney disease on dialysis. It is also approved for bone disease medical treatment of patients with secondary hyperparathyroidism. For patients with primary hyperparathyroidism in whom surgery is contraindicated, bone disease medical treatment consists of antiresorptive therapy to address low bone mass.
Renal Osteodystrophy
This complex bone condition is the result of chronic kidney failure. The bone disease medical treatment of renal osteodystrophy depends on the stage of kidney disease. It also depends on the type of bone abnormality associated with it. In patients with chronic renal disease, preventing renal osteodystrophy involves implementing dietary restrictions on protein and phosphates. It also requires supplementation with oral calcitriol (1-25-dihydroxy vitamin D). In addition, the patient must ensure adequate dietary intake of vitamin D and calcium.
One study showed that patients on hemodialysis who were treated with paricalcitol, a vitamin D analog, had lower mortality rates than patients treated with calcitriol. Patients with end-stage renal disease are treated with dialysis to address uremia (high blood urea nitrogen). An increasing number of patients on dialysis are undergoing renal transplants. However, following transplantation, immunosuppressive therapy is necessary to prevent organ rejection. These immunosuppressive drugs can aggravate bone loss, leading to osteoporosis.
Post-transplant osteoporosis can be managed by giving immunosuppressive agents and corticosteroids at the minimum effective dose. This is part of the bone disease medical treatment program. Furthermore, kidney transplant patients can also be treated with established osteoporosis treatments such as bisphosphonates.
Paget’s Disease of Bone
This condition is associated with an excessive amount of remodeling in localized areas of bone. Both old bone resorption and new bone formation are increased. Bone disease medical treatment primarily consists of bisphosphonate treatment to decrease resorption and reduce the rate of bone turnover. Several bisphosphonates, such as alendronate, tiludronate, risedronate, and etidronate, are approved treatments for Paget’s disease. The drugs are prescribed at higher doses than osteoporosis treatment.
Excessive bone turnover in Paget’s disease causes skeletal pain. Bisphosphonates are frequently able to decrease this pain by decreasing the amount of alkaline phosphatase. Another bone disease medical treatment for Paget’s disease, somewhat less effective than bisphosphonates, is subcutaneous or nasal calcitonin. It should be noted that PTH is not prescribed to patients with a diagnosis of Paget’s disease.
Bone Metastases
Secondary deposits of cancer in bone occur with a number of malignancies. They are associated with a high rate of morbidity and mortality. Prostate cancer, breast cancer, and multiple myeloma feature prominently in the list of primary cancers that are associated with secondary bone deposits. The most common symptom of bone metastases is often severe intractable pain. In particular, prostate cancer and bone metastases have a special relationship. As many as 90 percent of patients with advanced cancer of the prostate gland develop bone metastases. These are clinically significant with osteoblastic remodeling leading to morbidity and mortality. They require bone disease medical treatment.
The metastatic lesions associated with breast cancer are frequently both osteoblastic and osteoclastic in nature. The effect of spread of multiple myeloma to bone involves rapid bone loss with severe intractable pain, fractures, and an increase in serum calcium levels. All of these require bone disease medical treatment. Osteolytic lesions scattered throughout the axial skeleton are often the leading cause of morbidity and mortality in multiple myeloma patients. These lesions are the result of osteoclastic activity and bone resorption in the vicinity of myeloma cells. In addition, myeloma cells produce local factors that block the formation of new bone, thus leading to extensive bony destruction.
Bone Disease Medical Treatment for Metastases
Treatment for metastases consists primarily of bisphosphonates. This is a class of drugs which strongly inhibit bone resorption. Studies have shown that bisphosphonates can significantly reduce the morbidity associated with secondary spread of advanced breast cancer. In experimental models, bisphosphonates reduce bone metastases from breast cancer cells. The FDA has granted approval to a second-generation bisphosphonate, pamidronate, as a bone disease medical treatment of osteolysis associated with breast cancer. In addition, a third-generation bisphosphonate, zoledronic acid, is an approved treatment for bone metastases.
In animal models, prostate and breast cancer-associated bone pain responds to osteoprotegerin. This is a protein which is an inhibitor of bone resorption. It should be noted that despite reducing the skeletal morbidity of bone metastases, studies have shown that treatment with bisphosphonates does not improve survival rates in cancer patients. The current understanding of bone metastasis pathophysiology is limited. Further investigations are needed to improve bone disease medical treatment and limit the damage caused by these lesions.
Osteogenesis Imperfecta
This is an inherited skeletal disorder. It is the result of a variety of genetic defects that result in low bone mass and brittle bones that are prone to fracturing. Thus, the mainstay of bone disease medical treatment for OI patients is the prevention and treatment of fractures. Bisphosphonate therapy has shown encouraging results. Patients with OI require a team of healthcare professionals, including orthopedists, physical therapists, and rehabilitation specialists, to manage the disease.
Therapies for Bone Diseases
There is convincing evidence that adequate nutrition and a healthy lifestyle with regular physical activity are beneficial to bone health. This prevents the need for bone disease medical treatment. Pharmacotherapy is available to slow down bone loss and increase the formation of new bone. Nonetheless, “cures” for osteoporosis and most other bone disorders remain elusive. Certain curative drugs are available, but their use is limited by expense, difficulty of administration, and/or intolerable side effects. Future research needs to focus on developing so-called “ideal” therapies that address these issues.
Finding Effective Therapies
In addition, investigators must determine the relative risks and benefits of different types of drugs used to treat different populations of patients. This will help identify the best candidates for bone disease medical treatment with bisphosphonates, SERMs, and anabolic agents. Further research is needed to determine the most effective pharmacotherapy for patients with hip fractures. Comparisons of single-drug regimens and combination therapies as well as different doses, dosing schedules, and methods of administration will help health professionals understand what works best in which type of patient.
Improving Compliance with Bone Treatment
Scientists also need to develop methods to encourage compliance with pharmacotherapy and prevent fractures in the community setting, i.e., outside the realm of a confined clinical trial. This is critical for the success of any bone disease medical treatment. The effect of different doses, longer and shorter regimens, and spacing of treatment, as well as the utility of surgical interventions such as kyphoplasty and vertebroplasty must be investigated in more detail. Finally, a deeper understanding and more effective therapies are needed for bone disorders such as renal osteodystrophy, primary hyperparathyroidism, and osteogenesis imperfecta.
X-ray CE
We offer a range of online CE courses for radiologic technologists who wish to fulfill their CEU requirements for the ARRT® or other registries. Browse our shop and purchase e-courses which can be completed conveniently online. You can also check out our free radiology CE page for any current offers. Our bone densitometry course is ideal for DXA operators and will earn 23 CE credits in one shot.