Radiography Shielding Tips
Inadiquate patient shielding during radiography can contribute to increased patient dose. For radiologic technologists, shielding is particularly important to protect anatomic areas of the patient near the exposure field, but should not interfere with obtaining diagnostic information.
Gonadal shielding devices are used during diagnostic x-ray procedures to protect the reproductive organs from exposure to the primary beam. They should be used when the gonads are within approximately 5 cm of a properly collimated beam. In these cases, gonadal shielding should always be used unless it will compromise the diagnostic value of the examination. gonadal shielding should not be used as a substitute for an adequately collimated beam. Adequate collimation is the first step in gonadal protection.
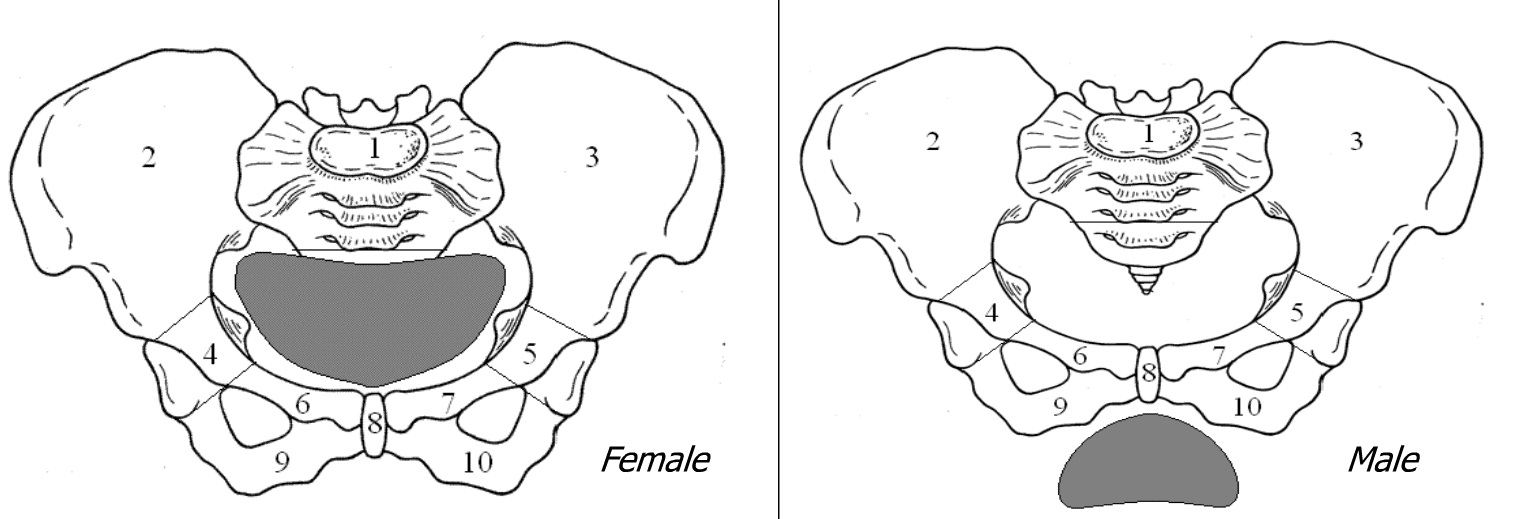
Female reproductive organs receive about three times more exposure during a given radiographic procedure involving the pelvic region than do the male reproductive organs. This obviously is because of the location. However, gonadal exposure for both men and women may be greatly reduced through the application of appropriate shielding. For female patients, the use of a flat contact shield (containing 1 mm of lead) placed over the reproductive organs reduces exposure by about 50%. Primary beam exposure for male patients may be reduced as much as 90% to 95% when the gonads are covered with a contact shield (also containing 1 mm of lead).
Since most pelvic x-rays and some hip x-rays expose the gonads to the primary beam, shielding is required as long as the shielding doesn’t cover an area of clinical interest. The regulations are clearly outlined in CFR – Code of Federal Regulations title 21 – subpart C – Radiation Protection Recommendations – Sec. 1000.50 Recommendation for the use of specific area gonad shielding on patients during medical diagnostic x-ray procedures.
Shielding for hip and pelvis can be tricky. Most of the time, male gonad shields are not a problem. However ovarian shielding on females is occasionally not possible without blocking essential anatomy. This is magnified when the patient is uncooperative such is often the case with children. However difficult it may be, our best effort is required. It’s appropriate to consult the ordering provider on a case by case basis about shielding when it appears that it will interfere and whether or not attempting to shield is worth the risk of a repeat exam.
Female gonads are considered protected when the shield covers the middle two thirds of the pelvic basin in the transverse plane and completely covers the pelvic basin from the symphysis pubis to the sacrum in the longitudinal plane. For protection of the ovaries of a female patient, the shield should be placed approximately 1 inch medial to each palpable anterior superior iliac spine.
External anatomical landmarks on the patient can be used to guide placement of a testicular or ovarian shield. For example, when a male patient is in the supine position, the symphysis pubis can be used to guide shield placement over the testes.
If not placed correctly, the shield can obscure anatomical structures that may need to be included in the image. The loss of this essential anatomic information in the image can result in a repeat projection. If the projection is repeated, patient dose will increase as a consequence. For this reason, the technologist must take care and double check that the shield is correctly placed before an exposure is made.
Additionally, there is a psychological factor to shielding that is often overlooked. Simply placing a shield on the patient’s lap can help the patient, or parents of pediatric patients, to feel more comfortable with the procedure even if the shield is not necessary. With very little reason not to shield, it’s a good practice to always shield unless there is a good reason not to.
Flat contact shields are made of lead strips or lead-impregnated materials. Usually they are a vinyl covered strip of lead or a strip of lead incased inside a nylon cover such as an apron. These shields may be placed directly over the patient’s reproductive organs or secured to the patient with Velcro straps or tape. These shields are most effective for exams where the patient is in a recumbent position. Lap shields and half-shields can help protect the patient’s gonads. Specially shaped shields can be helpful for male gonads, female breasts, and thyroids. Flat contact shields are not well suited for upright positions. lf the flat contact shield is used during a fluoroscopic examination, it needs to be under the patient since the x-ray tube is located under the radiographic table.
Shadow shields are made of a radiopaque material that hangs over the area of clinical interest to cast a shadow in the primary beam over the area that needs to be shielded such as the patient’s reproductive organs. The beam-defining light must be accurately positioned to ensure correct placement of the shadow shield. When the shield is correctly positioned, it provides protection from the radiographic beam as efficiently as the contact shield. If the shield is not correctly positioned, a repeat examination may be necessary, resulting in an additional radiation exposure that will increase patient dose. The shadow shield is not suitable for use during fluoroscopy because no localizing light field exists and the field of view is usually moved about during a study. Another advantage of shadow shields is that they protect the patient’s modesty by minimizing the need for a radiographer to palpate the patient’s anatomy for shield placement.
Shaped contact shields are made of radiopaque material contoured to enclose the male reproductive organs. They are inserted in disposable or washable athletic supporters. The cuplike shape of the shield permits it to be placed comfortably over the scrotum and penis whether the patient is recumbent or not. These are good for AP, oblique, and lateral projections may be obtained with maximal gonadal protection. This shield is also suitable for use during fluoroscopic examinations. However, they are not good for PA projections because the shield covers the anterior surface of the reproductive organs.
Radiosensitive organs and tissues other than the reproductive organs may be selectively shielded from the primary beam during an exam. Contact lens shields for the lens of the eye can reduce or eliminate exposure to that highly sensitive area. Particularly sensitive breast tissue may be shielded by using a clear lead shadow shield. This shielding is of vital importance in providing protection during juvenile scoliosis examinations. Radiation dose to the breast of a young patient may be further reduced by performing the scoliosis examination with the radiographic beam entering the posterior surface of the patient’s body instead of the anterior surface. The use of the PA projection results in a lower radiation dose to the anterior body surface, reducing the dose to the patient’s breasts.
Radiographers should follow department guidelines for proper shielding. Shielding is a fundamental radiation safety practice. A best practice in radiography is the use of lead shielding for anatomic parts that are adjacent to the x-ray field.
Get more information about radiologic technologist continuing education credits here
