Quantitative Computed Tomography (QCT) and Osteoporosis
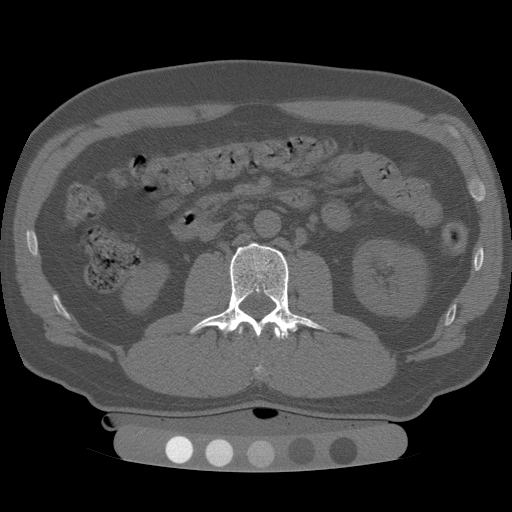
Quantitative computed tomography (QCT) is a medical technique that measures bone mineral density (BMD) using a standard X-ray Computed Tomography (CT) scanner with a calibration standard to convert Hounsfield Units (HU) of the CT image to bone mineral density values. Quantitative CT scans are primarily used to evaluate bone mineral density at the lumbar spine and hip.
Figure 1 (above): A QCT of spine showing five fixed reference densities in the calibration device under the patient’s back that help adjusting CT machine and calculating accurate bone mineral density (BMD).
Bone Densitometry: Evaluating Osteoporosis
Bone densitometry is a crucial branch of orthopedics focused on evaluating osteoporosis through the measurement of bone density. Several imaging techniques are available today to accurately determine bone mass density (BMD), with quantitative computed tomography (QCT) being the most advanced and precise method. Another commonly used technology for measuring bone density is dual-energy X-ray absorptiometry (DXA).
Limitations of DXA
While DXA is widely recommended, it has limitations in accurately assessing osteoporosis:
- Two-Dimensional View: DXA provides a 2-D or “areal” view of bone density.
- Inability to Differentiate: DXA cannot distinguish between trabecular (soft bone) and cortical (hard bone) density changes.
This limitation can lead to less accurate assessments because trabecular and cortical bones have distinct density characteristics and changes.
Advantages of QCT
QCT offers significant advantages over DXA by facilitating three-dimensional volumetric measurement of bone:
- 3-D Volumetric Measurement: Allows for separate analysis of interior trabecular or spongy bone tissue and the dense cortical bone wall.
- Accurate Detection: QCT can accurately detect changes in trabecular bone density, crucial for early recognition of osteoporosis.
- Effective Monitoring: Highly effective in monitoring the therapeutic effects of osteoporosis treatments.
“By providing a true volumetric measurement, QCT can accurately detect changes in trabecular bone density, which is particularly useful for the early recognition of osteoporosis.”
Performing High-Quality QCT Scans
To perform high-quality QCT scans, follow these guidelines:
- Ensure proper patient positioning to obtain accurate measurements.
- Calibrate the QCT machine regularly for precise imaging.
- Use standardized protocols to maintain consistency in measurements.
Key Differences Between QCT and DXA
Understanding the key differences between QCT and DXA can help in selecting the appropriate imaging technique for osteoporosis evaluation:
- Measurement Technique: QCT provides three-dimensional volumetric measurements, while DXA offers a two-dimensional areal view.
- Bone Type Distinction: QCT can distinguish between trabecular and cortical bones, whereas DXA cannot.
- Accuracy: QCT is more accurate in detecting true bone density and early changes in trabecular bones.
This article delves into the fundamentals of bone densitometry, exploring the use of both DXA and QCT in this field. It outlines the procedure for performing high-quality QCT scans and highlights the key differences between QCT and DXA. Understanding these differences and the capabilities of each technique is essential for healthcare professionals aiming to accurately diagnose and treat osteoporosis.
Bone Mineral Density (BMD)
Bone mineral density (BMD) is a critical measurement that quantifies the amount of bone mineral per unit area or volume of bone tissue. Several techniques are employed to measure BMD, including:
- Conventional X-ray radiography
- Dual-energy X-ray Absorptiometry (DXA)
- Quantitative Computed Tomography (QCT)
- Quantitative Ultrasonography
Among these, DXA and QCT are the most frequently used methods due to their accuracy and reliability.
Osteoporosis and Affected Areas
Osteoporosis, although a systemic disease, predominantly affects specific areas of the body such as the:
- Spine
- Hip
- Distal radius
- Proximal femur
Standard BMD measurement procedures involve the use of X-ray radiation. As the X-ray beam passes through the body, bone tissue absorbs some of the radiation, while the remainder passes through and is captured on a radiosensitive plate. The amount of radiation that escapes through the body and is detected correlates directly with the bone mineral density. This measurement is expressed either as mineral per area (g/cm2) or mineral per volume (mg/cc).
Understanding T Scores and Z Scores
The primary BMD result is then converted into T scores and Z scores to aid in the diagnosis of osteoporosis.
- T Score: Compares a patient’s bone density to that of a healthy young adult of the same sex and ethnicity, representing the standard deviation from this reference value. A T score between -1 and -2.5 indicates osteopenia, while a T score of -2.5 or lower confirms osteoporosis.
- Z Score: Compares a patient’s BMD to the average BMD of individuals of the same age and gender. This score provides additional context by showing how the patient’s bone density compares to others in their age group. The risk of osteoporosis doubles with each point deviation below the standard Z score.
“Each point deviation from the average T score significantly increases the risk of fractures.”
Techniques for Measuring BMD
Both T scores and Z scores can be derived from DXA and QCT scans. Here are some key points:
- DXA: Commonly used for its efficiency and ability to measure bone density in central (spine and hip) and peripheral (wrist) sites.
- QCT: Offers the added benefit of providing three-dimensional imaging, allowing for the separate evaluation of trabecular (spongy) and cortical (dense) bone, enhancing the detection of early changes in bone density.
Understanding the differences and applications of these techniques is essential for accurate diagnosis and effective management of osteoporosis. For more detailed guidelines and insights into BMD testing and the interpretation of T and Z scores, explore our comprehensive resources at BMD Testing Guidelines in Young and Middle-Aged Adults.
Dual-energy X-ray Absorptiometry (DXA)
Dual-energy X-ray absorptiometry (DXA) is the most widely used method for measuring bone mineral density (BMD) in the evaluation of osteoporosis. This technique is favored for its accuracy, low radiation dose, and ease of operation. DXA employs two X-ray beams at different energy levels, which helps to overcome the limitations of radiation absorption by soft tissue, providing a clearer assessment of bone mass.
Principle Behind DXA
The principle behind DXA involves using two X-ray beams with distinct intensities to pass through bone and soft tissues. Key points include:
- Dual Beams: Two X-ray beams at different energy levels.
- Absorption Analysis: Analyzes the difference in absorption between the two beams to determine bone density.
- Proportional Absorption: The amount of X-ray absorbed by the bone is directly proportional to the bone mass present.
This data is then converted into T scores and Z scores, which are used to compare an individual’s bone density with that of a healthy reference population.
Applications of DXA
DXA is extensively used for both diagnosing osteoporosis and evaluating the risk of developing osteoporosis, particularly in older adults:
- Age Recommendations: For women, DXA scans are typically recommended starting at age 50, and for men, at age 60.
- Common Sites Scanned: The lumbar spine, proximal femur (hip), and distal radius (wrist).
These sites are critical as they are the most prone to osteoporotic fractures.
DXA Scan Results
The results of a DXA scan are expressed in terms of bone mineral content per area, usually in grams per square centimeter (g/cm2). These measurements are crucial for determining bone health and the effectiveness of any ongoing treatment for osteoporosis:
- T Score: Compares the patient’s bone density to the peak bone density of a healthy young adult of the same sex, indicating the risk of fractures. A T score between -1 and -2.5 suggests osteopenia, while a T score of -2.5 or lower confirms osteoporosis.
- Z Score: Compares the patient’s bone density to the average bone density of individuals in the same age group, providing additional context for the diagnosis.
“A T score between -1 and -2.5 suggests osteopenia, while a T score of -2.5 or lower confirms osteoporosis.”
Importance of DXA
DXA is an essential tool in the management of osteoporosis, offering precise and reliable measurements of bone density. It is integral for:
- Diagnosing the condition
- Assessing the risk of fractures
- Guiding effective treatment strategies
For more detailed information on DXA and its application in bone health, explore our resources at DXA Technologist Advice for Patients.
Quantitative Computed Tomography (QCT)
Quantitative Computed Tomography (QCT) is a sophisticated radiological technique utilized for bone densitometry. It employs a CT scanner to assess bone density and evaluate the effectiveness of bone mass therapy. This advanced imaging method allows for detailed analysis of bone health, particularly in critical areas such as the spine and hip, which are essential for diagnosing and monitoring osteoporosis.
3D Imaging Advantage
QCT provides a three-dimensional (3D) view of the scanned areas, offering a more comprehensive evaluation compared to two-dimensional methods like DXA:
- Multiple X-ray beams are projected from different angles around the body.
- The collected data is combined to create a detailed 3D image of the bone structures.
This capability allows radiologists to assess variations in bone density across different regions of the axial skeleton and hip, highlighting areas more severely affected by osteoporotic changes.
Trabecular vs. Cortical Bone Measurement
One of the key advantages of QCT is its ability to separately measure the density of trabecular (spongy) bone and cortical (hard) bone:
- Trabecular Bone: Found primarily in the spine and ends of long bones, it is more metabolically active and more susceptible to osteoporosis.
- Cortical Bone: Denser and less affected by osteoporotic changes.
“By providing detailed measurements of trabecular bone density, QCT facilitates early diagnosis of osteoporosis, enabling timely intervention and treatment.”
Radiation Exposure
QCT involves a higher radiation dose than DXA but significantly lower than that of a standard CT scan. The radiation dose used in QCT is carefully optimized to balance image quality and patient safety.
- Hounsfield Units (HU): Measurements obtained during a QCT scan are expressed in HU, which quantify the X-ray attenuation of the scanned tissues.
- Milligrams of Hydroxyapatite per Cubic Centimeter (mg/cc): These HU are then converted into mg/cc, providing a precise representation of bone mineral density (BMD).
Applications in Osteoporosis Management
QCT is instrumental in both the diagnosis and management of osteoporosis. It offers a reliable method for:
- Monitoring the progression of the disease
- Assessing the effectiveness of therapeutic interventions
Its ability to provide detailed 3D images and differentiate between trabecular and cortical bone makes it an invaluable tool in the comprehensive assessment of bone health.
Quantitative Computed Tomography (QCT)
Quantitative Computed Tomography (QCT) is a powerful tool used to evaluate bone health, particularly in distinguishing existing fractures, assessing the risk of vertebral fractures, and monitoring age-related bone loss. QCT’s ability to provide high-resolution images makes it invaluable for analyzing the trabecular structure of bones with a level of precision unattainable by other methods.
Measuring Bone Mineral Density (BMD)
QCT accurately measures the bone mineral density (BMD) of the lumbar spine using standard CT scanners equipped with specialized software:
- Peripheral QCT (pQCT): Small-bore CT scanners assess bones like the forearm or lower leg.
- Precise Measurement: pQCT devices evaluate bone density and structure in appendicular sites, crucial for measuring both trabecular and cortical bones.
“QCT’s high-resolution images provide a detailed analysis of the trabecular structure of bones, offering precision unattainable by other methods.”
Advantages of QCT
QCT offers several significant advantages over traditional methods like DXA:
- Separate Assessment: QCT allows for the separate assessment of cortical and trabecular bones, providing a more detailed and accurate picture of bone health.
- True Volumetric Density: QCT results represent true volumetric density in milligrams per cubic centimeter (mg/cc), unlike the areal density provided by DXA.
- Accuracy: QCT results are free from errors caused by degenerative disk disease and aortic calcification, which can affect DXA measurements.
Peripheral Measurements
Peripheral QCT (pQCT) devices provide detailed information on the mass, distribution, and geometry of bone materials:
- Enhances assessment of bone strength
- Helps determine the bone’s ability to withstand mechanical stress, such as bending and torsional loads
QCT vs. DXA
Despite DXA being widely recommended for bone densitometry, QCT is increasingly used due to its distinct advantages:
- High-Resolution Imaging: QCT’s high-resolution images offer a detailed analysis of bone health.
- Enhanced Precision: QCT provides precise measurements of trabecular and cortical bones.
- Reduced Measurement Errors: QCT results are not affected by conditions like degenerative disk disease and aortic calcification.
Disadvantages of QCT
While QCT offers many advantages, there are some drawbacks to consider:
- Higher Radiation Exposure: QCT involves a higher level of radiation exposure compared to DXA, necessitating careful consideration of the benefits versus risks.
- Cost: The cost of QCT is significantly higher than that of DXA, which can be a limiting factor in its widespread adoption.
“Despite these challenges, the increasing accuracy and detailed insights provided by QCT make it a valuable tool in the comprehensive evaluation of bone health.”
Clinical Benefits of QCT
Despite its disadvantages, QCT remains highly beneficial in clinical settings for several reasons:
- Precise Measurement: QCT provides accurate measurements of bone density, crucial for diagnosing and monitoring osteoporosis.
- Bone Type Differentiation: QCT’s ability to differentiate between trabecular and cortical bones enhances its diagnostic capability.
This makes QCT particularly valuable for clinical evaluations where detailed and precise bone health assessments are critical.
How to Obtain Appropriate Results from QCT
Obtaining accurate results from Quantitative Computed Tomography (QCT) requires meticulous preparation and execution by the radiologic technologist. Here’s a step-by-step guide to ensure precision and reliability in your QCT scans:
Preparation and Review
- Review Physician’s Request: Thoroughly examine the physician’s request and the patient’s medical records, including clinical indications and any specific instructions for the QCT examination.
- Leverage Previous Scans: Utilize results from previous non-contrast CT scans of the abdomen or pelvis for osteoporotic evaluation whenever possible to spare the patient additional radiation exposure.
Patient Communication and Comfort
- Explain the Procedure: Clearly explain the QCT procedure to the patient to ensure they are comfortable and aware of what to expect.
- Address Claustrophobia: Discuss any claustrophobia concerns beforehand to alleviate anxiety and ensure a smoother scanning process.
Proper Positioning
- Correct Positioning: Position patients with their hands above their head and ensure the scan table is clear of pillows and other positioning aids.
- Remove Metal Objects: Ensure all metal objects within the scan area are removed to prevent artifacts in the imaging.
Quality Assurance
- Routine Quality Checks: Perform routine quality checks at every operational step to ensure consistency and accuracy.
- Standardized Protocols: Follow standardized radiological guidelines and specific manufacturer protocols to minimize radiation dose while producing high-quality images.
- Calibration: Regularly calibrate the CT scanner to prevent drift in CT numbers, ensuring reliable and reproducible results.
Consistent Scan Protocols
- Follow-Up Examinations: Review previous reports and select the same vertebrae for subsequent scans to maintain consistency and reproducibility.
- Lateral View: Include a lateral view of the lumbar spine in QCT spine examinations, focusing on the position and size of the region of interest (ROI).
- Exclude Certain Vertebrae: Exclude vertebrae with fractures, deformities, metastases, or those affected by prior surgery unless a thorough review confirms the absence of any lytic or blastic processes.
“By following these guidelines, radiologic technologists can ensure accurate and reliable assessments of bone mineral density, essential for diagnosing and monitoring osteoporosis and other bone-related conditions.”
For further insights and detailed information on QCT and its applications in bone densitometry, explore our resources on advanced radiological techniques and bone health management.
Learn more about advanced radiological techniques and bone health management at CE4RT.