Radiation Dose in Modern Diagnostic Radiology
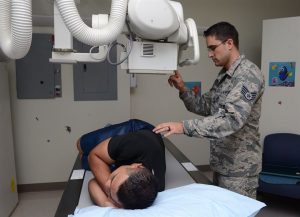
Over the past several decades, the use of ionizing radiation in medical imaging has increased dramatically. This has resulted in a substantial increase in the radiation dose humans are exposed to. In 1950, approximately 25 million radiographic and fluoroscopic exams were performed. This number skyrocketed to nearly 300 million by the mid-2000s. In the 1980s, only 15 percent of all artificial radiation exposure was on account of medical imaging; by the mid-2000s, this figure had risen to almost 50 percent.
Although natural background radiation exposure has not changed substantially, human exposure to radiation has increased by more than 30 percent in the past few decades, mainly due to an increase in the number of medical imaging examinations performed. This increase has been driven primarily by CT scans and interventional cardiology procedures. It is also noteworthy that occupational exposure to radiation occurs primarily in the medical and aviation professions. To learn more about the history of medical imaging, read our paperless e-course which is worth 2 ARRT® credits.
Growth in Radiation-Based Imaging Studies
The tremendous growth in the use of radiation-based medical imaging has improved diagnosis and disease management, but it has raised concerns about the risks of ionizing radiation. The use of digital technology in radiology examinations has the potential to lower the radiation dose, but it can also increase the dose delivered to patients if used incorrectly. Dose savings of 50 percent or more are possible with digital imaging technology compared to film-screen radiography. The magnitude of risk from ionizing radiation is related to dose. If radiation protection in digital radiology is not carefully regulated, millions of people could receive radiation exposure without concurrent benefit. For this reason, international and national bodies legislate patient radiation exposure from medical examinations.
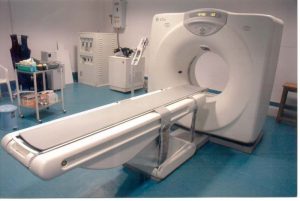
What are the most commonly performed radiographic examinations?
In the late 1990s, approximately 26 million CT examinations were performed in the United States. A decade later, this figure had risen dramatically to 70 million. It is thus evident that CT imaging is the biggest contributor to medical radiation exposure. In addition to the abovementioned modalities, external beam radiotherapy also exposes patients to radiation. However, this modality is unique because only a small percentage of the population is exposed, consisting of individuals battling life-threatening illnesses such as cancer.
The approximate percent contribution of various imaging modalities to the total medical radiation exposure of patients is as follows:
- 49 percent of radiation exposure is from computed tomography examinations
- 26 percent of radiation exposure is from nuclear medicine studies
- 14 percent of radiation exposure is from interventional fluoroscopy procedures
- 11 percent of radiation exposure is from conventional radiography/fluoroscopy
Efforts to Reduce Unnecessary Radiation Exposure
To ensure patient radiation safety, campaigns such as Image Gently and Image Wisely advocate actions to reduce unnecessary radiation exposure in all age groups. Appropriateness criteria recommendations are available to help with clinical decision making. The ICRP has proposed diagnostic reference levels (DRLs) to provide a benchmark for patient exposure. If DRLs are consistently exceeded, it calls for an investigation and corrective action. The NCRP has defined certain radiation values known as substantial radiation dose levels (SDRLs). SDRLs are trigger levels that indicate the need for followup measures.
In other words, SDRLs serve as alerts to medical professionals that potential harm may have occurred. In such cases, the patient should be informed to remain alert for signs and symptoms of cutaneous radiation injury. If the SDRL threshold is exceeded, the reason (clinical necessity) for this should be recorded on the patient’s chart. In addition, the patient’s radiation history should be carefully documented to avoid cumulative exposure. Furthermore, to comply with regulatory requirements, it may be necessary to report the radiation dose and any injuries that occurred.
Quality Assurance Program
Within every hospital system, a quality assurance program and ongoing feedback is necessary to ensure the radiation protection of patients, staff, and visitors. The quality assurance peer review committee is responsible for evaluating any unusually high doses and statistical trends. The committee typically consists of a qualified medical physicist and radiology interventionists. The committee evaluates safety matters related to sentinel events, i.e., when there is an unexpected radiation exposure involving serious injury or death. It is worth noting that medical errors and sentinel events are not the same thing – not all errors cause sentinel events and not all sentinel events are due to errors.
A skin dose of more than 15 Gy is classified as a sentinel event, although the timeframe over which this dose is delivered is not clearly defined. If a tissue reaction occurs after a fluoroscopically-guided procedure, for example, it is necessary to carefully evaluate procedure justification, dose optimization, procedure complexity, patient-specific factors, the timeframe over which the dose was delivered, and the severity of tissue injury.
Role of the Radiologic Technologist in Radiation Protection
Radiation protection in digital radiography takes the combined efforts of radiologists, technologists, medical physicists, and equipment manufacturers to ensure high quality images are captured at reasonable doses. Technological advances have helped to optimize radiation dose. For example, valuable diagnostic information can be obtained from a PET/MR scan with a smaller radiation dose compared to a PET/CT exam. In addition, as mentioned before, the dynamic range of digital systems is wider than film-screen systems. This means operators have the opportunity to vary exposure level and lower patient dose without influencing image contrast.
As long as the reduced signal-to-noise ratio is acceptable and the image quality is good enough to answer the clinical question, digital radiography offers the opportunity for dose saving. However, operators should be aware that above a certain dose level, changes in the dose do not produce an observable effect in image contrast. Therefore, operating the equipment in this exposure range can lead to unnecessarily high patient radiation doses. Digital radiological examinations should be tailored to provide the required diagnostic information and not necessarily to deliver the lowest exposure. Digital radiography systems have the flexibility to offer this customization.
Radiation-Induced Tissue Damage
Experts have studied how low doses delivered over a prolonged period of time and high doses delivered over a shorter timeframe affect humans. The damage from low doses of radiation can be repaired by the body’s natural defense mechanism. Therefore, when the dose is low, the probability of radiation-induced cancer is proportional to the dose. At high doses, on the other hand, the cell’s internal mechanisms may not have a chance to repair the damage and the probability of cancer depends on the square of the dose. At very high doses, the probability of cancer drops down again because the cells die before they become cancerous.
The effect of radiation dose on the probability of cancer is demonstrated by the dose response curve. Localized doses of radiation are less damaging than whole-body exposure to the same dose. Interestingly, experts assume there is no threshold dose below which the risk of radiation-induced cancer is zero. This may or may not be true, but it does underline the importance of a cautious approach whereby all unnecessary exposure to radiation should be avoided.
Acute vs Chronic Exposure
Radiation exposure that occurs over a short timeframe, such as within a day, is called acute. When exposure to radiation is a one-time event and a high dose is involved, the symptoms appear quickly within days to weeks. In contrast, radiation exposure delivered over a longer period of time, such as months or years, is termed chronic. When exposure to radiation is over the long-term and a low dose is involved, the effects of this cumulative dose may become evident only decades later in the form of radiation-induced cancer. Latent period is the time between exposure to radiation and manifestation of effects (for example, cancer).
Effect of Dose
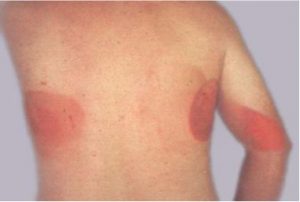
When a very high dose (more than 100 rem) is delivered over a short period of time (few hours), such as during a radiation accident, outright cell death occurs. For this reason, very high acute radiation exposures are lethal, and as such, the individual may die within days to weeks. About half the people exposed to a whole-body dose of around 500 rem will die within a month if they do not receive any treatment. Doses of more than 700 rem delivered over a few hours will likely cause death within a few weeks of exposure. However, when the radiation exposure is spread out over weeks, the human body can survive doses as large as 1000-2000 rem. Acute localized irradiation, usually from exposure to the primary X-ray beam, can lead to radiation burns. The severity of the cutaneous radiation injury depends on the dose, the duration of exposure, the energy of the beam, and the sensitivity of the individual.
Radiosensitivity of Tissues
At lesser doses, the damage to the chromosomes affects the ability of the cell to reproduce. It is not surprising then that tissues with rapidly reproducing cells are most affected by acute doses of radiation. These highly-mitotic tissues are called radiosensitive tissues or organs. Examples of such self-renewing radiosensitive tissues include the gonads, skin, blood-forming cells, and the lining of the digestive tract. When we look at the functions of these tissues, it is easy to predict the symptoms of acute radiation exposure, commonly known as radiation sickness. Radiation sickness manifests with signs and symptoms such as diarrhea, nausea, vomiting, bloody vomiting, mouth ulcers, spontaneous bleeding, fever, dizziness, headache, fatigue, erythema, skin sloughing, hair loss, and infections. The effects of ionizing radiation on the human body are broadly classified as deterministic, stochastic, and heritable.
ARRT® CE Credits
We have many online courses for ARRT® category A credits for X-ray continuing education. See our general instructions section to learn how to purchase a course, navigate our website, and complete your CE requirement in a few easy steps. We have a 24-credit course that will allow you to fulfill your biannual requirements in one shot.
Visit here to know about radiologic technologist ceu
