Dual Photon X-ray Absorptiometry: Equipment and Procedure
Dual photon X-ray absorptiometry (DPA) technology is now largely of academic interest. However, learning about it can help DXA operators understand the benefits of DXA and why it has become the gold standard in bone densitometry.
DPA Technology for Bone Mineral Density
Dual photon X-ray absorptiometry (DPA) machines contain an isotope, gadolinium-153, as the source of photons. In contrast, dual-energy X-Ray Absorptiometry (DXA) devices incorporate an X-Ray tube. Therefore, dual photon X-ray absorptiometry is actually a misnomer. DPA machines produce a photon beam with two distinct energy levels of 44 keV and 100 keV. The energy that is absorbed more by soft tissue is subtracted from the energy that is absorbed more by bone to determine the mineral content (density) of bone.
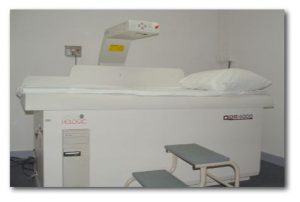
DPA Equipment
Dual photon X-ray absorptiometry equipment consists of a collimated gadolinium source and scintillation detector assembly mounted in opposing geometry over a full-body table. An interface connects the system to a computer which generates an image on a display. DPA scans can be performed on fracture-prone areas such as the spine and hip. They can also be done on the entire skeleton to calculate the total calcium content in the body. Routinely, L1-L5 vertebrae in the spine are scanned with the region of interest being L2-L4. The scan takes 30-45 minutes to complete.
Preparation for DPA Scanning
Prior to the procedure, the patient’s age, sex, height and weight is recorded. If the patient has taken any contrast material or undergone any radioactive studies within 3-5 days, the dual photon X-ray absorptiometry test should be rescheduled. All metal objects are removed from the scan area since they can make the results invalid. The patient should be questioned about prior operations on the lumbar spine because deformities, laminectomy, and bone grafts can all falsify bone mineral values. Deformed or postsurgical spinal levels are excluded from the study for accurate results. Note is made of the medications the patient is taking because estrogen, steroids, calcium, vitamin D, and fluoride are known to affect the mineral content of bone.
DPA Positioning
The patient is positioned supine and the lumbar spine is centered on the imaging table. Elevating the legs helps to flatten the lower back and separate the lumbar vertebrae. The dual photon X-ray absorptiometry device features automatic edge detection software, but the operator can manually override this to correct errors. During interpretation of a hard copy image, the physician compares the image to a recent radiograph of the lumbar spine to exclude any compression fractures, degenerative changes, or scoliosis from the region of interest because this can result in a false bone mineral value. The patient’s bone mineral content is compared to normal values adjusted for age and gender with consideration given to race as well.
To maintain the accuracy and precision of dual-photon absorptiometry machines, strict quality control must be performed. This includes scanning substances that simulate bone to check the scanner and detector function. Ashed bone is the absolute standard and reference point against which computer results are compared for accuracy and reproducibility.
Dual Photon Absorptiometry vs DEXA
Like any imaging modality, dual photon X-ray absorptiometry has some advantages and some limitations. Studies have compared the accuracy, precision, reproducibility, and limitations of DPA and DEXA. Comparison of DPA and DXA can pose problems. In general, the limitations of DPA instruments are that they produce lower resolution images than DXA. The scanning time with DPA is 20-40 minutes, which is considerably longer than DXA (under 7 minutes). In addition, DXA offers better precision and more accurate measurement of area.
Due to greater accuracy in area measurement, the BMD result with DXA is consistently lower and more accurate than the result obtained with DPA. Moreover, the gadolinium source in dual photon X-ray absorptiometry machines decays over time. This affects the accuracy of the results. Replacement of the photon source costs thousands of dollars, adding to the cost of machine maintenance. For these reasons, DPA is rarely used these days and has been largely replaced by X-Ray-based DXA technology. DXA has gained acceptance in clinical and research applications as the method of choice for measuring bone mineral density.
Affordable X-ray CE Courses Online
To earn ARRT®-recognized CEUs and complete the biannual requirements for continuing education, radiologic technologists can purchase one or more of our e-courses. These courses are a quick and convenient way to complete X-ray CE from the comfort of home. For example, our e-course on Radiography of the Upper Extremities is good for 24 CE credits and allows you to complete your requirements in one shot. Browse our selection of e-courses and buy the type and number of credits you need.
Get details about radiography continuing education credits here.